Host factors in TB
- Read more about Host factors in TB
- Log in to post comments
Host factors in TB disease are various factors/attributes of the host(person who is developing TB disease/infection).
The various host factors are as follows:
Content Status where content has been uploaded and published on LMS.
Host factors in TB disease are various factors/attributes of the host(person who is developing TB disease/infection).
The various host factors are as follows:
Mycobacterium tuberculosis (M. tuberculosis) belonging to the family Mycobacteriaceae cause Tuberculosis (TB).
These are rod shaped bacilli and require oxygen to survive (aerobic bacteria).
The following characteristics of these bacilli help them to survive in human body for a long time and resist the action of drugs:
Predictive values are important for a diagnostic test because they tell how truly a test result reflects the truth. Positive predictive value (PPV) and negative predictive value (NPV) are true positive and true negative results of a diagnostic test, respectively. In other words, if someone receives a certain diagnosis by a test, predictive values describe how likely it is for the diagnosis to be correct.
Positive Predictive Value
PPV is the percentage of patients with a positive test who actually have the disease.
In 1993, the World Health Organisation devised the Directly Observed Treatment Strategy (DOTS) and recommended all countries to adopt it. It called for Nationally coordinated, high-quality TB services, which were priority for improving advancing and sustaining the fight against TB.
The DOTS strategy is based on five components as shown in the below figure.
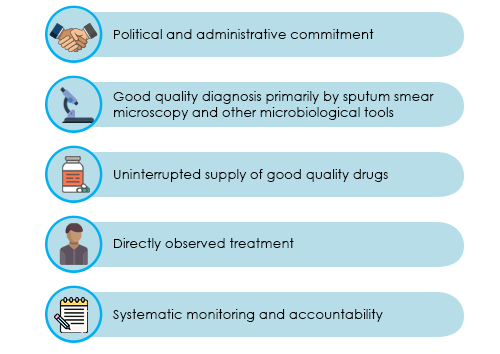
Figure: Components of the DOTS Strategy
Resources
Patients suffering from microbiologically confirmed pulmonary TB (PTB) constitutes the most important source of infection.
Following are the risk factors that increase the chances of developing TB disease in an individual:
![]()
Figure: Risk factors for developing active TB
Resources:
Specificity is the test’s ability to correctly designate a subject without the disease as negative.
Specificity of a test is the percentage of true negatives out of all subjects who do not have a disease or condition.
Simply, specificity is the proportion of people without disease correctly diagnosed as negative by a test. In other words, it is the ability of the test or instrument to obtain normal range or negative results for a person who does not have a disease.
The formula to determine specificity is the following:
Sensitivity is the proportion of true positive tests out of all patients with a condition.
In other words, it is the ability of a test or instrument to yield a positive result for a subject that has that disease. A test that is 100% sensitive means all sick individuals are correctly identified as sick, i.e., there are no false negatives. Importantly, as the calculation involves all patients with the disease, it is not affected by the prevalence of the disease.
Prevalence is an epidemiological measure of the proportion of a population with a disease or a particular health condition at a specific point in time (point prevalence) or over a specified period of time (period prevalence).
Tuberculosis (TB) prevalence refers to the number of people with TB that are present in a particular population at a given time. Calculation of the TB prevalence rate is shown in the figure below.
Mycobacterium tuberculosis, gets its name from the disease it causes (tuberculosis) and the properties of the bacterial order/ family it is classified under. Below is the description of the origin of both the words "Tuberculosis" and "Mycobacterim".