Biosafety in TB Laboratories
ContentWhat is Biosafety?
Biosafety is safe handling and containment of infectious microorganisms and hazardous biological materials.
Why Biosafety?
Infections which are obtained through laboratory or laboratory-related activities are known as Laboratory Acquired Infections (LAI). These infections are major occupational health hazards and are a cause of concern for the safety of the staff working in laboratories.
Routes of entry of LAI
There are multiple routes of entry and transfer of toxic material through the body and its transfer to various organs and systems.
The most predominant routes of LAI are:
- Nose - Inhalation of infectious aerosols
- Mouth - Ingestion or exposure through mouth pipetting or touching mouth or eyes with contaminated fingers or contaminated object
- Skin and mucous membrane:
- Spills and splashes onto skin and mucous membranes
- Parenteral inoculations with syringes or other contaminated sharps
- Animal bites and scratches from research laboratories or activities
Biosafety guidelines are prepared to promote:
- Safe microbiological practices
- Safety equipment and facility safeguards for reducing LAIs
- To protect public health and the environment
Biosafety in Tuberculosis TB laboratory (lab)
In a TB lab, the primary risk for infection transmission is the aerosol contaminated with TB bacilli when:
- TB patients walk into the laboratory for specimen collection or other testing and may be a source of droplet infection if they cough during laboratory visits
- Procedures such as centrifugation, vortexing, and vigorous shaking generate significant aerosols that are biohazardous
Key points to consider for M. TB as a biological hazard are given in the table below.
MYCOBACTERIUM TUBERCULOSIS (M. TB) AS BIOLOGICAL HAZARD
RISK FACTORS
Pathogenicity
M.TB exposure may lead to infection
5-10% of infected persons will develop TB disease
Primary route of transmission
Inhalation
Stability
Tubercle bacilli can remain viable for extended periods in the environment
Infectious dose
As little as 10 bacilli can infect humans
Effective Vaccine (for adults)
No vaccine is available for adults
Effective treatment for strain susceptibility to different medicines
Yes
Effective treatment for MUltiple Drug Resistant (MDR), Extensively Drug Resistant (XDR) strains
Yes, but more difficult to treat than susceptible strains
Standards for TB Lab Biosafety
- Standards are prepared based on the recommendations from the WHO expert group in 2012.
- Standards use a procedural approach for the assessment of risk.
- It establishes minimum requirements necessary to ensure biosafety during TB microscopy, culture, drug-susceptibility testing (DST) and molecular testing in different countries and epidemiological settings.
Resources
Kindly provide your valuable feedback on the page to the link provided HERE
Precautions for Using the Biosafety cabinet [BSC]
ContentThere are certain Do’s & Don'ts that should be followed while operating the Bio Safety Cabinet (BSC).
Do’s:
- Read the Standard Operating Procedure (SOP) before starting the work inside the BSC.
- Carry out functionality tests (smoke test, pressure gauge monitoring) before use, and maintain a record at installation and after the maintenance of BSC.
- Check that the sash is at normal operating height (READY state). Adjust the chair height so that your face is above the sash.
- Always use good microbiological practice when working inside the BSC.
- Disinfect work surface, interior walls and interior window surface before and after work.
- Maintain the log sheet after every run of BSC and perform the maintenance activity as required.
Don’ts:
- Never work in the cabinet with the ultraviolet light ON.
- BSC should not be used with the sash window above the design opening mark.
- Perform all the work on or over the work surfaces; avoid working over or placing items on the front grill or blocking the front or rear grills.
- To reduce turbulence, avoid rapid movement while working.
- Avoid unnecessary movement of hands and arms in and out of the cabinet.
- Open flames (Bunsen burners) should never be used inside the BSC; open flames actually create turbulence that disrupts the air flow and damages the filters.
- Never operate the cabinet when any alarms are activated.
Resources
Kindly provide your valuable feedback on the page to the link provided HERE
Biosafety Cabinet [BSC] Class I
ContentThe Biosafety Cabinet (BSC) or microbiological safety cabinet is an enclosed, ventilated laboratory workspace for safely working with materials.A Class I BSC is defined as a ventilated cabinet for personnel and environmental protection.Class I BSCs protect workers but do not protect work products (such as specimens or cultures) against contamination because unsterilized room air is drawn over the work surface.
- Class I biosafety cabinets are typically used to either enclose specific equipment like centrifuges or for procedures like aerating cultures that might potentially generate aerosols.
- Biosafety cabinets of this class are either ducted (connected to the building exhaust system) or unducted (recirculating filtered exhaust back into the laboratory).

Figure: BSC Class I Airflow Diagram - In the Class I BSC, the room air is drawn in through the opening that also allows the entry of the operator’s arm during work.
- The air inside the cabinet then takes in the aerosol particles that may have been generated and moves it away from the operator towards the HEPA filter.
- The air moving out of the cabinet is thus, sterilised via the HEPA filters before its discharge to the environment either:
- Into the laboratory and then to the outside of the building through the building’s exhaust system; or
- To the outside through the building’s exhaust system; or
- Directly to the outside.
- In this way, the cabinets protect the operator and the environment from the aerosols but not the sample.
Resources
Biosafety Cabinet [BSC] Class II Type A2
Biosafety Cabinet [BSC] Class III
Cleaning and Maintenance of the Biosafety cabinet [BSC]
ContentThe daily maintenance of the Bio Safety Cabinet (BSC) should be performed by lab staff and include:
- Surface decontamination of the work zone
- Cabinet power-up alarm verification
- Removal of unnecessary items from the BSC
- Flow check (inflow and downflow velocity)
- Smoke pattern test
- Entry in the logbook (shown in Table 2)
The weekly maintenance tasks to be performed by lab staff are:
- Surface decontamination of the drain pan
- Surface cleaning of fluorescent (FL) and ultraviolet (UV) lamps
- Front sash cleaning
Biosafety cabinets must undergo certification:
- At the time of installation
- Whenever they are moved
- Following any repairs or filter changes
The BSCs also require regular (annual) maintenance to ensure proper functioning.
Delaying maintenance or using underqualified personnel to conduct maintenance can put laboratory workers at risk.
Annual Maintenance - To be performed by an external agency
Parameters verified:
- Down flow and inflow velocities
- Particle count test
- Airflow smoke patterns
- Poly Alpha Olefin (PAO) test for High Efficiency Particulate Air (HEPA) filter integrity
The table 1 below summarizes the description of maintenance tasks to be performed and their frequency:
Table 1: Maintenance Tasks to be Conducted on the BSC
Description of task to be performed
Maintenance to be carried out every
Day
Week
Month
Quarter
Annually
1. Surface decontaminate the work zone
Yes
2. Cabinet power-up alarm verification
Yes
3. Decontaminate the work surface and interior surfaces with 5% phenol followed by 70% alcohol
Yes
4. Note the manometer’s reading, indicating any fall in pressure flowing through the HEPA filter
Yes
5. Thoroughly surface decontaminate the drain pan
Yes
6. Check the paper catch for retained materials
Yes
5. Clean the exterior surfaces of the cabinet
Yes
7. Check all service fixtures for proper operation
Yes
8. Inspect the cabinet for any physical abnormalities/ malfunction
Yes
9. Re-certification
Yes
10. Change UV-lamp
8000-9000 hrs. of use
Table 2: Maintenance Log Sheet
Date
Time of use
Cumulative duration of use
Cumulative duration of use of UV lamps
Visual alarm
Sound alarm
Smoke test
Airflow
m/s
(for class II BSC)
Observation
Operator’s
Sign
Change UV lamps after XXX hours of use (according to manufacturer's recommendations)
Resources
Kindly provide your valuable feedback on the page to the link provided HERE
Biosafety Requirements in the LPA Lab: Refrigerated Centrifuge Use
ContentThe refrigerated centrifuge is used in the mycobacteriology laboratory for concentrating bacterial cells, following the processing of sputum or other specimens. It is also used for spinning down reagents from walls of containers. The temperature maintained within the refrigerator centrifuge is 4°C to reduce the percentage of mycobacteria killed due to heat generated during centrifugation. The required G force is 3000 x g (not RPM).
Essential Features of the Refrigerated Centrifuge
- Swinging Bucket Rotor: The component that is rotated by the drive system and holds the containers being centrifuged. It is air and liquid-tight. It allows for longer distance of travel which allows better separation, and it is easier to withdraw or decant the supernatant without disturbing the pellet
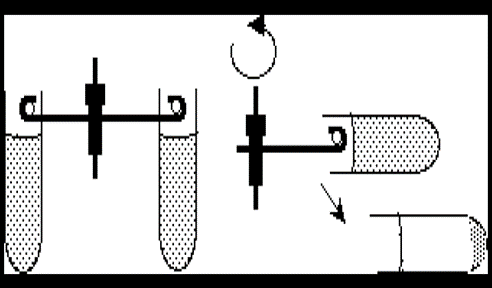
Figure 1: Advantage of the swing bucket in the centrifuge
- Sealed Safety Centrifuge Cups:
- Safety cups protect laboratory staff by providing containment of any aerosols that are produced during centrifugation, especially if tubes break (see Figure 2)
- Safety cups must be opened inside the biosafety cabinet (BSC)
- Safety cups have a silicone- coated rubber O-ring that provides an air-tight seal
- These seals must remain coated with silicone so that seals stays air-tight
Before use, it is important to inspect all the components.
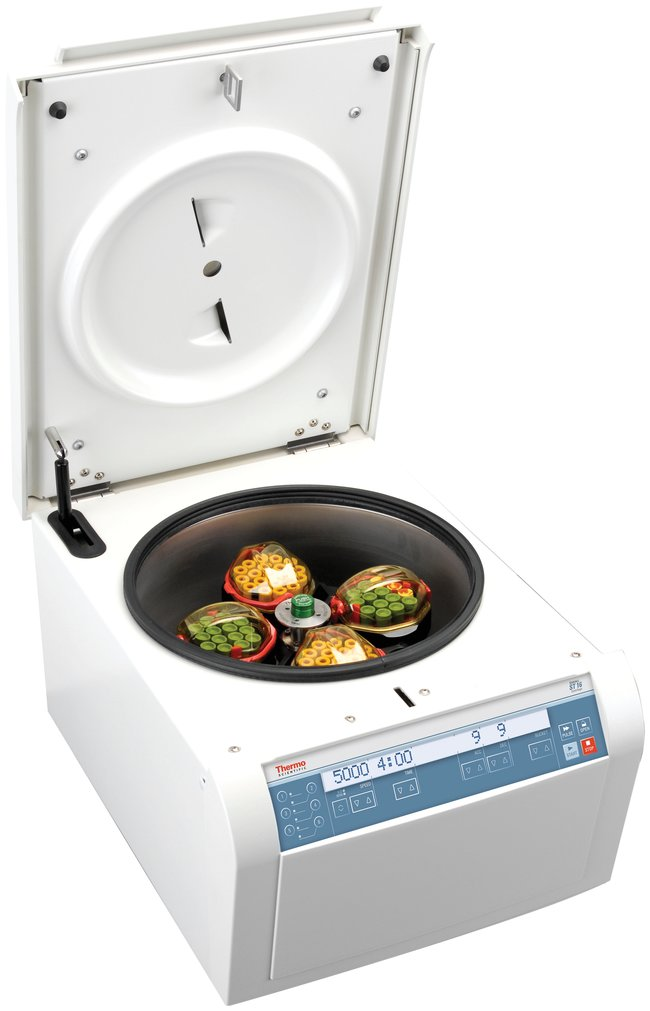
Figure 2: Refrigerated Centrifuge

Figure 3: Rotor and Centrifuge Cup (indicated by arrow) in a Refrigerated Centrifuge
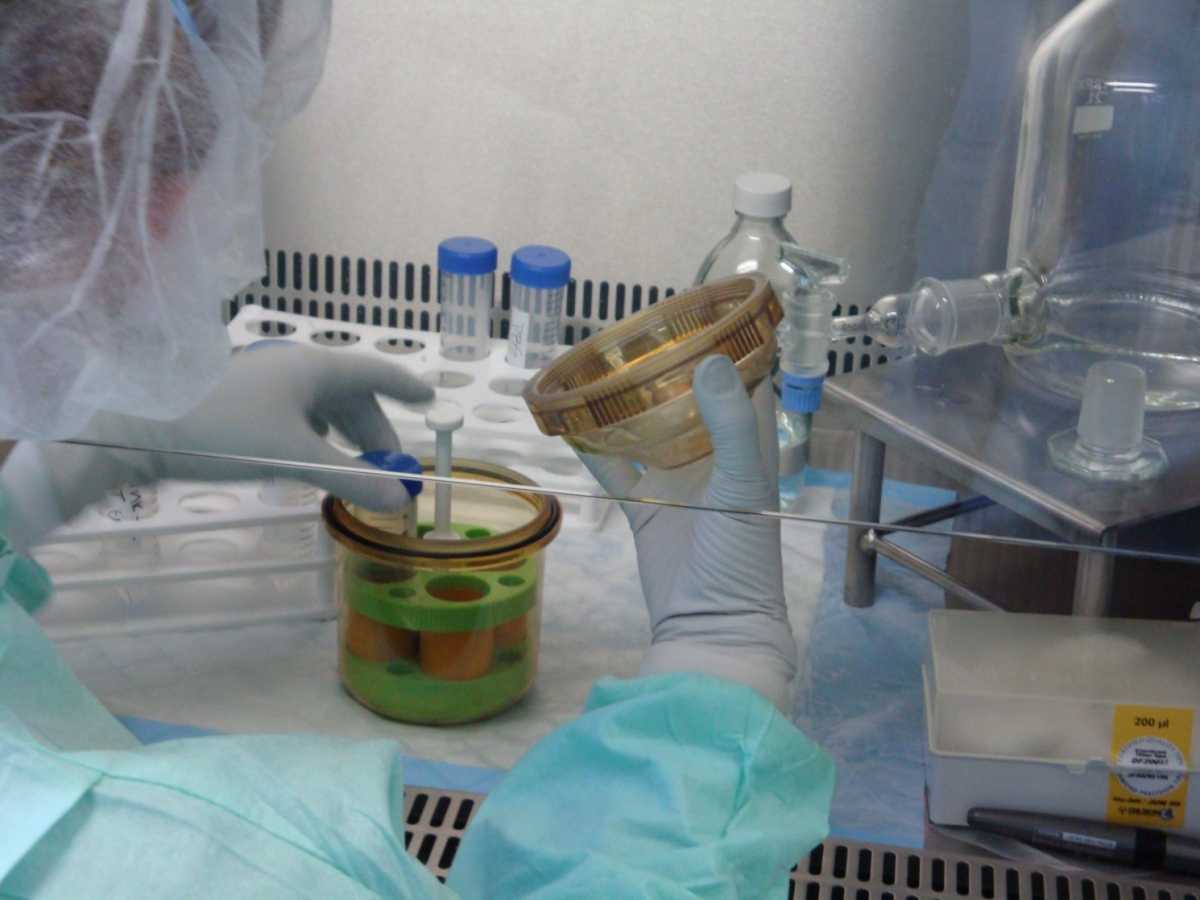
Figure 4: Safety bucket in use
Principle of Procedure
- A centrifuge is intended to separate particles in a liquid by sedimentation. Dense particles sediment first, followed by lighter particles.
- In a TB laboratory, centrifuges are used for the sedimentation and concentration of tubercle bacilli within liquefied sputa or body fluids (usually urine).
- To obtain a high sedimentation efficiency of 95%, i.e. 95% of bacilli recovered in the sediment and only 5% of bacilli still in suspension to be discarded with the supernatant, it is necessary to maintain 3,000 g for 15-20 minutes.
- The high speeds and time used to achieve effective sedimentation efficiency leads to heat build-up in the centrifuge and the specimen.
- To prevent cell death due to overheat, the use of a refrigerated centrifuge model, operated at 18-20°C, is recommended.
Refrigerated Microcentrifuge
- Provides high-speed centrifugation up to 13,000 rpm
- Use microcentrifuge tubes with a capacity of 1.5 to 2.0 ml
- Fixed angle rotor with a lid
- Rotor can be removed from the centrifuge chamber

Resources
Kindly provide your valuable feedback on the page to the link provided HERE
How to Use Refrigerated Centrifuges
ContentPrinciple of procedure
- A centrifuge separates particles in a liquid by sedimentation. Dense particles sediment first, followed by lighter particles
- To obtain a high sedimentation efficiency of 95%, it is necessary to centrifuge the TB specimens at 3,000 g for 15-20 minutes
- The high speed and time used to achieve effective sedimentation efficiency lead to heat build-up in the centrifuge and the specimens. To prevent cell death due to overheating, the use of a refrigerated centrifuge is recommended
How to use refrigerated centrifuges?
Select type of tube, based on:
- G force used for swing-out bucket
- Time of centrifugation
- Temperature
- Compatibility with specimen
- Chemically inert
Visually inspect tubes
Do not use if tubes have:
- Cracks
- Scratches
- Chipped rims
Fill tubes only to the recommended volume
- Do not overfill tubes
- High g forces can drive liquid up to the cap and cause overflowing
Before using centrifuge
- Inspect the interior of the bowl for stains
- Inspect rotors and buckets for cracks and signs of corrosion
- Always check the silicon O ring for any wear & tear of the aerosol lid
- Check log book to ensure centrifuge is in good working condition
- Pre-cool centrifuge prior to use
Use of safety centrifuge
- Centrifuge load MUST always be balanced to avoid the risk of damage
- Add a balance tube with the same volume of water if processing an odd number of specimens
- Select the required time and g force or RCF
- Stop centrifuge immediately if any abnormal noise and/or shaking is noticed
- Never use the brake to stop a normal operating centrifuge for TB specimen processing
- ALWAYS open the sealed buckets inside the biosafety cabinet (BSC)
Microcentrifuge
- Always balance the rotor
- Use high-quality screw-capped tubes, which will not leak or break during centrifugation
- When using a microcentrifuge for DNA extraction, the microcentrifuge should be loaded and unloaded inside the BSC
- Remove and replace the rotor carefully
Resources
- World Health Organization laboratory biosafety manual 3rd edition, pgs 72-73
- Manufacturer's instructions
- Global Laboratory Initiative LC training module on Equipment slides 32-34.
Kindly provide your valuable feedback on the page to the link provided HERE
Revolutions per minute [RPM] vs Relative centrifugal force [RCF] in the Safety Centrifuge
ContentRevolutions Per Minute (RPM) and Relative Centrifugal Force (RCF) are important abbreviations used while using a centrifuge. However, these terminologies differ from each other.
RPM vs. RCF (g force)
- RPM indicates the speed at which the rotor is rotating.
- RCF is the term used to describe the amount of accelerative force applied to a sample in a centrifuge.
- RCF is measured in multiples of the standard acceleration due to gravity on the Earth’s surface (x g).
- This is why RCF and “x g” are used interchangeably in centrifugation protocols.
- The two variables that describe RCF are the radius and the angular velocity of the rotor, i.e., how wide the rotor is and how fast it is moving.
- RCF is more precise than RPM because the rotor size might differ, and RCF will be different, while the revolutions per minute stay the same.
Calculating RCF required from the known RPM value
Formula:
RCF = 1.1118 x 10 -5 x r x rpm2
r = radius in cm from the centrifuge spindle to the bottom end of the tube
RCF = desired centrifugal force
A nomogram, provided by the manufacturer, can be used to convert RPM to RCF value.
Resources
Kindly provide your valuable feedback on the page to the link provided HERE
Protocol for Cleaning and Maintenance of Refrigerated Centrifuge
ContentPeriodic maintenance of the refrigerated centrifuge is essential to ensure that the centrifuge is in optimum condition.
Daily Maintenance:
- For a refrigerated centrifuge that is turned off at the end of the day, open the top to allow the centrifuge chamber to dry (Figure 1).
- During the day, when the unit is under refrigeration, leave the top closed to avoid condensation and ice buildup.
- The centrifuge must not be used if the interior is hot, if unusual vibrations or noises occur, or if deterioration (corrosion of parts) is detected. A qualified service technician should be contacted.

Figure 1: Refrigerated Centrifuge with Open Top to allow the centrifuge chamber to dry
Weekly Maintenance:
- Autoclave metal parts OR soak them in a disinfectant (not bleach or alcohol) for 15 minutes, rinse with sterile water and air dry.
- Soak lids in freshly prepared 1% bleach for 5 minutes and rinse with 70% alcohol or sterile water.
- Checking the rotors and rotor bores visually for residue and corrosion (Figure 2).

Figure 2: Lids and Rotor Bores
Monthly Maintenance:
- Clean the centrifuge housing, rotor chamber, rotors and rotor accessories with a neutral cleaning agent, e.g., mild soap.
- Lubricate rotor threads with lubricant.
- Lubricate O-rings with lubricant supplied by the manufacturer.
- Clean plastic and non-metal parts with a fresh solution of 1% sodium hypochlorite (bleach), followed rinsing with sterile water.
Note: Each laboratory should maintain centrifuge usage record in a log book (Figure 3).

Figure 3: Centrifuge Usage Log Book
Annual Maintenance:
Full service should be provided by a qualified service technician, which may include the servicing of the following:
- Centrifuge brushes
- Timer
- Electrical components
- Leaks
- Speed
Good practices for centrifuge usage:
- Always carefully read the operating manual before the initial operation of the centrifuge.
- Run the centrifuge with samples that are symmetrically loaded in the aerosol tightened buckets and open the buckets in the Bio Safety Cabinet (BSC) after centrifugation is done.
- Routinely check the silicon O-ring for any wear & tear of the aerosol lid.
- Always use centrifuge tubes that will withstand the required centrifugation speed.
- Perform maintenance activity as required.
Practices to be avoided when using the centrifuge are:
- Moving or knocking during operation
- Running the unit when there is heavy noise from the machine
- Running with unbalanced sample load
- Running if there is any wear & tear with the O-ring of the aerosol lid
- Adding water to a specimen to balance tubes
- Stopping the running cycle
Resources
- World Health Organization Laboratory Biosafety Manual, 3rd edition, p72-73.
- Global Laboratory Initiative Training Package on LC.
Kindly provide your valuable feedback on the page to the link provided HERE
Quality Control Process of the Autoclave
ContentThe quality control process for autoclaves is important to prevent the transmission of infection.
It is done to ensure that sterilization or decontamination by the autoclave is up to the mark.
To ensure that biohazardous waste is properly decontaminated during autoclaving, the following procedures should be followed by laboratory personnel for quality control during autoclaving:
A. Use of Chemical Indicator
- With each load of sterilization, an autoclave tape needs to be used (Figure 1)
- The autoclave tape is a visible temperature sensitive chemical indicator, with stripes that change colour after proper autoclaving is done (Figure 2)

Figure 1: Autoclave tape used on the load of material to be sterilized

Figure 2: Change in the colour of strips in the autoclave tape before and after proper autoclaving
Note: Temperature sensitive autoclave tape is not sufficient on its own to indicate that the sterilization temperature (121ºC), is uniformly achieved throughout the chamber.
B. Biological Indicator (BI)
Biological indicators are used for checking the quality of autoclaving on a monthly basis, even if the autoclave has a paper printed monitoring system for autoclave effectiveness. The results need to be documented and kept for at least one year.
Principle of Biological Indicators
- Heat-resistant Geobacillus Stearothermophilus spores are used for autoclave efficiency testing
- After autoclaving, the autoclaved spore vial is incubated in a culture along with a non-autoclaved control vial at 56-60ºC
- The control biological indicator should yield positive results for bacterial growth and the autoclaved biological indicator should not show any growth (see Figure 3)
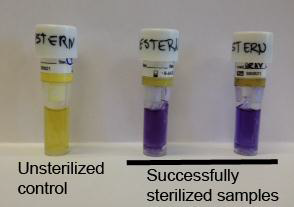
Figure 3: Showing effective use of the biological indicator
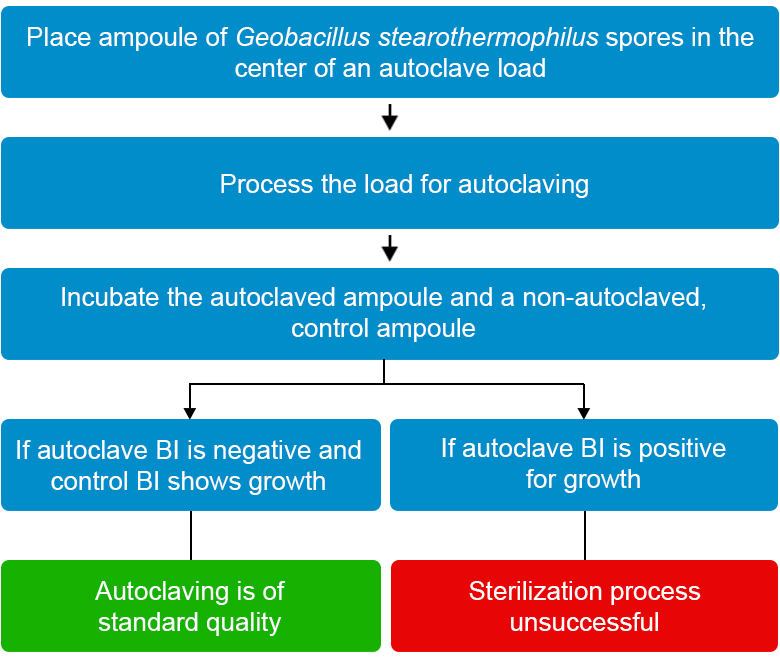
Figure 4: Steps to follow when using biological indicators
Reading and Recording
- Record details of the loading and of the autoclave’s operation in the autoclave logbook
- Incidents, accidents and/or mechanical problems must be recorded and reported to a supervisor immediately
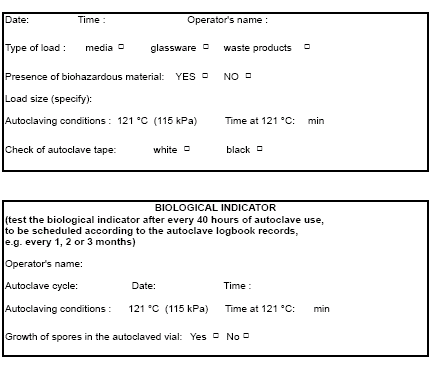

Figure 5: Autoclave Logbook
Resources
- Tuberculosis Laboratory Biosafety Manual, 2012, WHO.
- Mycobacteriology Laboratory Manual, April 2014, WHO.
- Autoclave Quality Assurance Program, Biosafety Manual, Boston University.
Kindly provide your valuable feedback on the page to the link provided HERE
Maintenance of the Autoclave in TB Labs
ContentAutoclaves are pretty simple to use but there are a few steps for better maintenance of an autoclave.
A. Daily Maintenance
- Check that the lid/ door gasket is clean. After each cycle of an autoclave, the lid must be cleaned properly.
- Check if there is any crack in the gasket. If a crack is there, the instrument should not be used.
- Check for leaks while the autoclave is running. If bubbles are coming out, it indicates leaking from autoclave. Such an autoclave must be tagged as “Not Approved for Infectious Waste” and should not be used.
- The autoclave and work area must be cleaned after every use.
- Sensor must be checked after every use and there should not be any damage to the sensor.
- The work area must be disinfected according to the Standard Operating Procedure (SOP) for disinfection.
B. Weekly Preventive Maintenance
- The drain strainer must be removed and cleaned, if necessary.
- Whenever the drain strainer is cleaned, its entry into the logbook must be done.
- The operator must check the operation of the pressure release safety valve to verify proper function. During this check, the operator must keep himself away from the release valve exhaust to prevent a burn injury.
Resources
Kindly provide your valuable feedback on the page to the link provided HERE
Common Problems and Troubleshooting Related to Autoclaves in TB Lab
ContentCommon Problems and Troubleshooting Related to Autoclaves in TB Lab
Table: Common Problems and Troubleshooting Related to Autoclaves in TB Lab
SR NO
PROBLEM
CAUSES
SOLUTION
1
Drain is clogged or exhaust taking more time than normal
There may be clogging of drain valve dust
- Clean the chamber
- Drain the filter
2
Scaling and salt deposition
- Cleaning is not proper
- There is moisture inside the instrument
- Exposure to chemicals like acids & detergents
- Cleaning must be improved and proper
- Check the sterilizer for efficient drying
- Store autoclave in a dry area
- Do not expose instruments to chemicals like acids and detergents. If exposure occurs, rinse thoroughly after contact
- Use only distilled water in the boiler
3
Liquid container caps blowing off
The sterilizer is exhausting too rapidly
Use slow exhaust cycle during autoclaving
4
When the door of the autoclave is open, the solution is still boiling
The door of an autoclave is opened too quickly
- Do not open an autoclave door until the temperature gauge is below 85⁰C and the pressure gauge is at "0"
- Do not touch or move a load, when the solution is boiling
5
Indicator of an autoclave shows sterilization not complete
- Load in an autoclave chamber may be too large, too dense, or improperly loaded
- The time provided for an autoclaving is not sufficient for the load
- Autoclave may be malfunctioning
- Don’t overload an autoclave with the material
- Load must be placed properly in an autoclave chamber
- Increase the time given for autoclaving
- Strips may need to be changed
6
Steam leakage
- The gasket may be worn out
- The door of an autoclave may be closed improperly
- The gasket needs to be changed
- The door needs to be closed properly
7
Chamber door won’t open
- There may be a vacuum in the chamber
- The door lock clutch of an autoclave may be jammed
- The gasket of an autoclave may be sticking to the door frame
- Follow manufacturer instructions properly during each cycle of autoclave
- Contact service engineer, if the problem persists
Resources
- Tuberculosis Laboratory Biosafety Manual, 2012, WHO.
- Mycobacteriology Laboratory Manual, April, 2014 , WHO.
Kindly provide your valuable feedback on the page to the link provided HERE
LPA Laboratory Equipment: Micro Pipettes
ContentUse of Micropipette
- Micropipette (Figure) dispenses and aspirates liquid (reagent, sample).
- IT is used in the DNA Extraction Room, Master Mix Room, Amplification Room and Hybridization Room to dispense reagents for Line Probe Assay (LPA).
- A micropipette should be dedicated to each room and labelled accordingly.
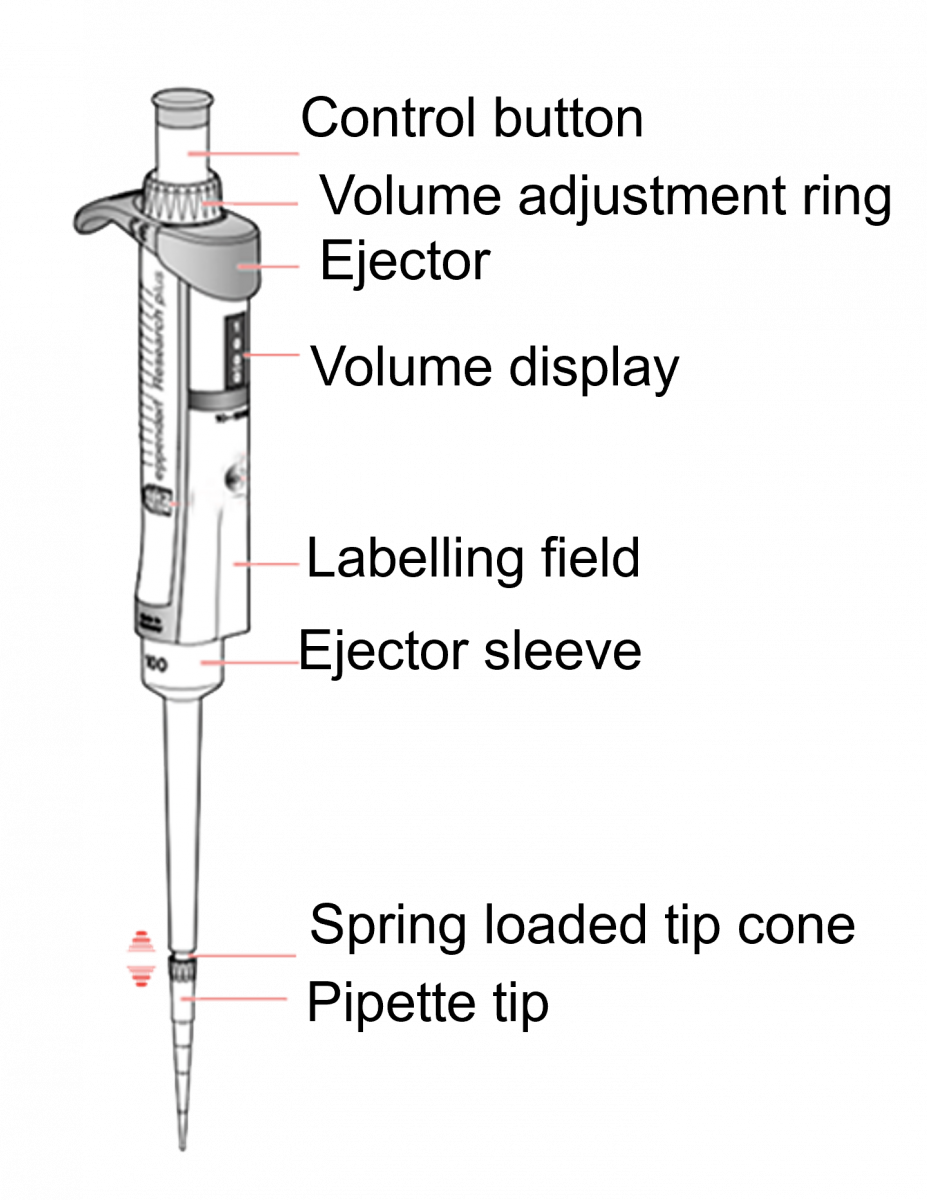
Figure: Micropipette
Cleaning:
- As per the manufacturer’s instructions
- Before and after every use wipe with 70% alcohol
Maintenance:
- Calibrated biannually
- To be done by a qualified service technician, which includes:
- Cleaning all parts
- Greasing of moving parts
- Checking function of all parts
- Calibration and validation using master calibration balance
Resources
Kindly provide your valuable feedback on the page to the link provided HERE
LPA Laboratory Equipment: Hot Air Oven
ContentUse of Hot Air Oven
- For heating non-explosive substances and objects
- For dry heat sterilization
- During DNA extraction step; kills Mycobacterium tuberculosis and partially lyses the cells at 95oC
Installation of the Hot Air Oven (Figure 1)
- The installation site must be flat and horizontal, and be able to reliably bear the weight of the appliance.
- Sufficient air circulation in the vicinity of the appliance must be guaranteed at all times.
- When installing, ensure that the distance between the wall and rear side of the appliance must be at least 15 cm.
- The clearance from the ceiling must not be less than 20 cm, and the side clearance from walls or nearby appliances must not be less than 5 cm.
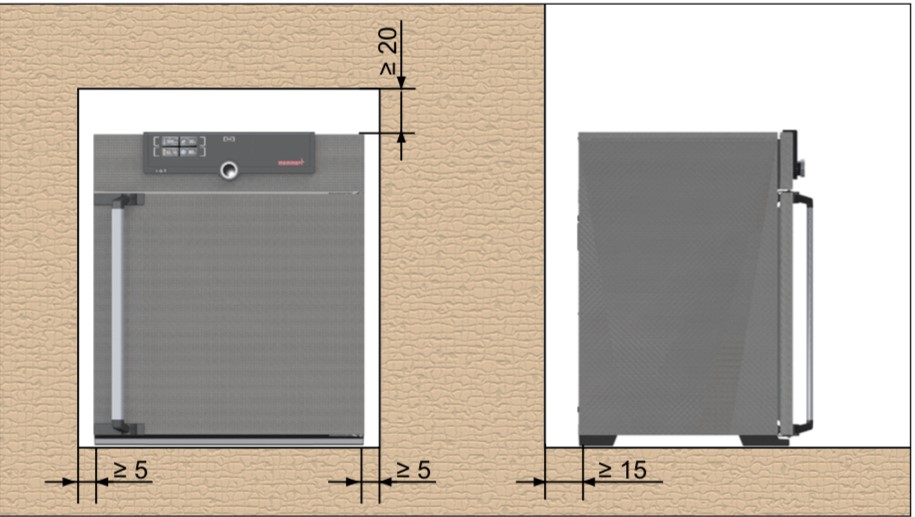
Figure 1: Clearance of the hot air oven to allow sufficient air circulation
Components of Hot Air Oven (Figure 2)
- Insulated chamber surrounded by an outer case containing electric heaters
- Fan
- Shelves
- Thermocouples
- Temperature sensor
- Door locking controls

Figure 2: Hot Air Oven Components
General Instructions for Maintenance
- Always switch off the appliance before any maintenance activity.
- Always record every maintenance activity performed.
Maintenance:
- Monitor temperature
- Immediately clean up with disinfectant if there is any spill
- Leave the rack in the oven
- Lubricate the door hinges and door lock systems for proper operation
Annual Maintenance:
Performed by a qualified service technician:
- Check temperature system
- Temperature distribution
- Noise level detection
- Overall operation and alarm function
Resources
Kindly provide your valuable feedback on the page to the link provided HERE
LPA Laboratory Equipment: Micro Centrifuge
ContentUse of Micro Centrifuge
- Designed for the separation of materials through sedimentation using centripetal force
- Used in DNA Extraction Room to concentrate specimens during processing
Components and Use (Figure)
- Air tight rotor – Provides containment for aerosols that may be released during centrifugation, loaded symmetrically
- Positions in air tight rotor - To evenly distribute centrifuge tubes on all rotor positions
- Capacity of centrifuge tubes = 1.5 ml
- Can run a maximum of 24 samples at a time
Note: Always refer to the user manual for operations.

Figure: Top and Inside view of a Micro Centrifuge
General Instructions for Maintenance
- Always switch off the appliance before any maintenance activity.
- Always record every maintenance activity performed.
Maintenance
- Clean the appliances with clean tissue paper
- Lubricate/oil the turners, hinge of the rotor, lid locking systems
- Disinfect the spills with appropriate disinfectants
- Disinfect interior and exterior assembly with 70% Ethanol
Annual Maintenance
Performed by a qualified service technician who:
- Inspects each part
- Calibrates and validates
- Monitors temperature
- Sensors speed
Resources:
Kindly provide your valuable feedback on the page to the link provided HERE
LPA Laboratory Equipment: Vortex Mixer
ContentKey Features of Vortex Mixer
It is used in the TB laboratory to mix specimens with decontamination solutions and to homogenize solutions of TB bacilli for DNA extraction and during the preparation of the PCR Master Mix.
- During the DNA extraction step:
- Growth from liquid culture is vortexed to break up clumped Mycobacterium tuberculosis
- Homogenize bacilli
- Mix specimens with decontamination solutions
- Gentle vortex is used to mix reagents in PCR master mix tube.
Most vortex mixers have variable speeds and can run continuously or run only when a tube is inserted in the rubber cup.
The mixer must always be placed on a level and stable surface. Vortex mixing generates aerosol, must be placed towards the back of the biosafety cabinet.
Components and Mechanism of the Vortex Mixer
The vortex mixer has the following components:
- Electric motor
- On and off switch
- Knob for increasing or decreasing the speed
- Cupped rubber piece mounted on the center

Figure: Components of the Vortex Mixer
As the motor runs, the rubber piece oscillates rapidly in a circular motion.
When a sample tube is pressed into the rubber cup or touched to its edge, the motion is transmitted to the liquid inside and vortex is created.
Maintenance of Vortex Mixer
- Before and after use, wipe it with 70% ethanol.
- Clean and replace the rubber cup as needed.
Resources
Kindly provide your valuable feedback on the page to the link provided HERE
- During the DNA extraction step:
LPA Laboratory Equipment: PCR Hood
ContentPolymerase Chain Reaction (PCR) hood is a workstation enclosed by three sides.
Use of Polymerase Chain Reaction (PCR) Hood:
- Used in the Master Mix Reagent Preparation and DNA Amplification Room
- Ultraviolet (UV) light (Figure) in PCR hood denatures nucleic acids
- Used to decontaminate reagents and equipment prior to PCR reaction
- Provides protection against exogenous DNA, contaminants or inhibitors from entering the reaction tubes
Figure: Components of the PCR Hood
- PCR Hood has UV light and recirculator fan with prefilters
- It is made of stainless steel, therefore easier to clean
- Always refer to the user manual for operating the equipment

General Instructions on Maintenance
- Always switch off the appliance before any maintenance activity.
- Always record every maintenance activity performed.
Maintenance
- Clean outer and inner surfaces with freshly prepared 1% sodium hypochlorite.
- Replace UV bulbs and filters according to manufacturer recommendations.
Resources
Kindly provide your valuable feedback on the page to the link provided HERE
LPA Laboratory Equipment: Thermocycler
ContentThermocycler is also known as Polymerase Chain Reaction (PCR) Machine.
Use of Thermocycler
Thermal cycler is used for amplification of nucleic acid by PCR.
The thermocycler should be placed in the amplification/ post-amplification area.
The features of a thermocycler are listed below.
Features of a thermocycler:
- High accuracy
- Programmable heat block
- Temperature controlled
- Time controlled

PCR is performed based on denaturation, amplification and annealing steps at different temperatures (Figure).
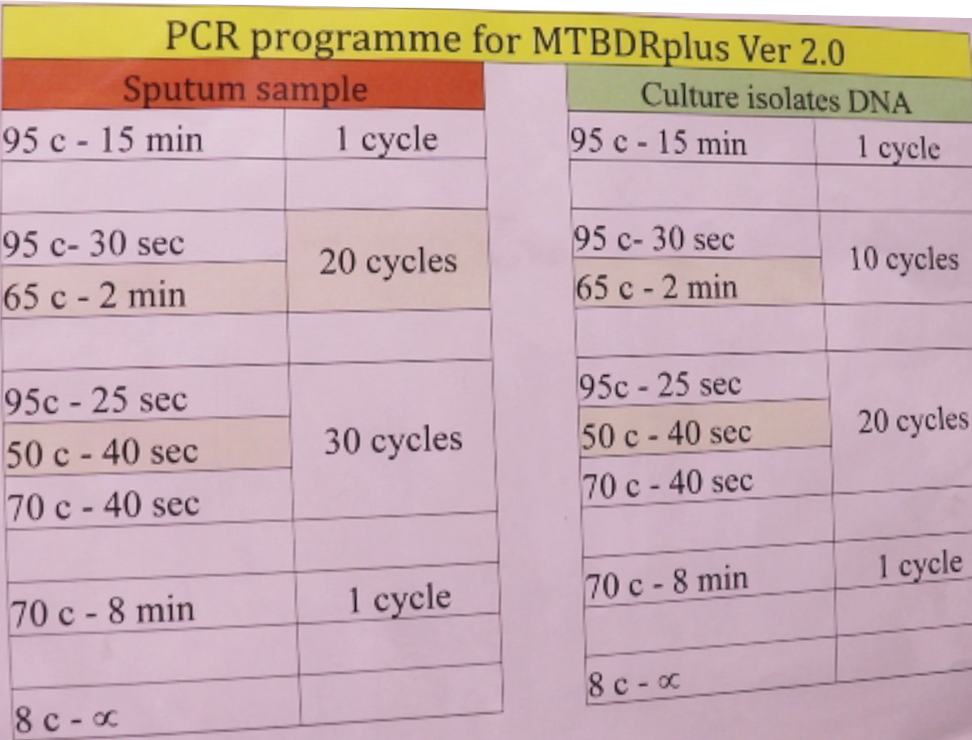
Figure: PCR Programme for MTBDR Plus Ver.2.0
General Instructions for Maintenance
- Always switch off the appliance before any maintenance activity.
- Always record every maintenance activity performed.
Annual Maintenance and Calibration
This is to be done by a qualified service engineer:
- Clean the exhaust fan assembly.
- Check all inbuilt switches.
- Temperature calibration and time validation with devices traceable to national and international standards.
- Validate the Peltier element efficiency by checking heating and cooling time, regimes and rates of block.
- Validate thermal block using PCR validation kit.
Resources
Kindly provide your valuable feedback on the page to the link provided HERE
LPA Laboratory Equipment: Water Bath
ContentIn the Line Probe Assay (LPA) lab, the water bath is used for warming reagents used in the Hybridization Room.
It is electrically heated and electronically controlled.
Components:
- Recessing push/ turn control for simple operation of the bath
- Visual temperature indication
- Push button to set desired temperature
- Electrically heated and electronically controlled
- Water trough
Installation of Water Bath (Figure):
- The unit must be placed on a horizontal, non-flammable sturdy surface.
- The vent openings must remain unobstructed.
- Minimum wall spacing on all sides is 80 millimetres.
- The minimum spacing from top of the bath to the next ceiling must be 750 millimetres.
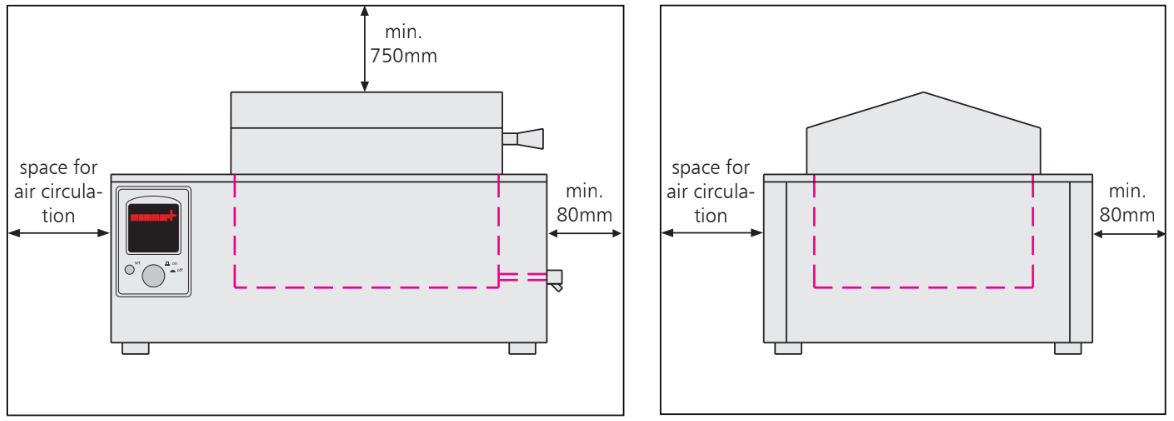
Figure: Spacing during Installation of Water Bath (Front and Side View)
Working with the Water Bath:
The heating positioned on three sides around the tank ensures a natural water circulation of the liquid inside, thus securing an optimal uniform temperature distribution.
- Vent openings must be unobstructed.
- The surface must be horizontal, nonflammable during installation.
General Instructions for Maintenance
- Always switch off the appliance before any maintenance activity.
- Always record the maintenance activity performed.
- Rusting objects must not come into contact with stainless steel bath tank.
- Rusting areas must be cleaned and polished immediately.
- Lubricate/ oil the hinge bolts from time to time.
- Replace distilled/ demineralized water and clean the water bath every week.
Annual Maintenance
- This is done by a qualified service technician
- Includes the calibration or validation of the temperature with a thermostat/ digital controller with devices traceable to National/ International Standards.
Resources
Kindly provide your valuable feedback on the page to the link provided HERE
LPA Laboratory Equipment: Twincubator
ContentUses of Twincubator in Line Probe Assay (LPA):
- Different steps of the hybridization (shown in figure below) and detection procedure with DNA strips in reverse blot hybridization assays.
- In the amplification/ post-amplification area.

Figure: Twincubator used in Hybridization
Features of Twincubator:
- Provides dry incubation
- Thermo-shaker
- Programmable
- Temperature and time-controlled features
- Pre-installed temperature profile for processing of the LPA tests
- Nine storage programs with up to 20 steps
- No. of samples run - 1 to 12, including one positive and two negative controls
- User friendly with minimum risk of contamination
Note: Always refer to the user manual for operation.
Maintenance:
- Always switch off the appliance before any activity.
- Always record every maintenance activity performed.
- Clean the housing of the instrument.
- The instrument must be protected from harsh chemicals.
- Clean the instrument immediately, if liquid enters the hybridization block.
- Perform preventive maintenance (temperature check) regularly.
Resources
Kindly provide your valuable feedback on the page to the link provided HERE
Laboratory Equipment: Thermometer
ContentThermometers are used to measure temperature. There are 4 types of thermometers used in line probe assay (LPA) laboratories:
- Electronic Thermo Hygrometer
- Alcohol Thermometer
- Digital Maxima – Minima Thermometer
- Dial Spring Thermometer
Electronic Max-Min Thermo-Hygrometer
It monitors the temperature and humidity, and has the following features:
- Recording of maximum/minimum humidity and temperature value automatically
- Alarm function
- Calendar function with months and years by pushing ADJ button (optional)
- Each thermometer is provided with a back stand and hanging hole
- Used in expert room and media preparation room

Glass Alcohol Thermometer
It is used for monitoring temperature of refrigerator, incubator, Walk-in Incubator (WII) and Walk-in Cold room (WIC). It has the following features:
- Temperature ranges from 0°C to +100°C
- Accuracy: ±1.0°C or better within the range 0°C to +70°C
- Resolution: ±0.5°C
- Sensor: Coloured alcohol in glass column
- Temperatures displayed in degrees Centigrade
- Casing is always non-corrodible plastics or metal case
- Easily readable centigrade scale

Digital Maxima-Minima Thermometer:
- Resolution: 0.1°C
- Accuracy: ± 0.1°C
- Precision: ± 0.2 % full scale
- Flexible probe (Preferably K type) Thermocouple, waterproof & Heat resistance cable/probe
- Measuring frequency: 3 measuring per second
- Display: Digital LCD display
Digital Maxima:
- Measuring range: -100°C to + 60°C
- It is used for calibration for -80 deep freezer, -20 deep freezer, refrigerator, WIC
Digital minima:
- Measuring range: 0°C to +300°C
- It is used for calibration for Incubator, Oven, WII, Autoclave, GT Blot, Twincubator, Thermocycler


Dial Spring Thermometer:
It is used for calibration for -80 deep freezer, -20 deep freezer, refrigerator, WIC.
- Temperature Range: +50°C to +300°C
- Accuracy: +1% Full Scale. Reading stabilization within 1 min
- Casting Material: Optically clear strong glass cover with stainless surface mount (highly resistance to corrosion)
- Type: Bimetallic dial thermometer
- Easily readable centigrade scale


Maintenance:
- Verify that all thermometers in the laboratory are accurately reflecting the temperature
- Always use calibrated thermometers
- Thermometers that are in use should be calibrated every 6 months and documented
Resources
Kindly provide your valuable feedback on the page to the link provided HERE
Fullscreen