Personal Protective Equipment [PPE] Use in TB Lab Settings
ContentWhat is Personal Protective Equipment (PPE)?PPE refers to physical barriers which are used alone or in combination to protect an individual's mucous membranes, airways, skin and clothing from contact with infectious agents, hazardous material, conditions or processes.
Components of PPE
- Protective clothing: Surgical gowns and laboratory (lab) coats
- Respiratory devices: N95 respirators
- Hand protection: Gloves
- Head protection: Headgear/ hair covers/ caps
- Foot protection: Shoe cover, safety shoes/ closed-toe shoes
- Eye protection: Safety glasses/ goggles, shields
PPE Hazard Assessment
- Evaluation of the PPE requirements for a specific activity or work environment is carried out by the lab director.
- For TB labs it is based on the risk assessment. PPE requirements will thus differ according to whether activities are classified as low risk, medium risk or high risk.
PPE Usage in Different Sections of the TB Laboratory
The table below lists the different PPE requirements for different sections of the TB lab.
Table: PPE usage in different sections of TB labs Section/ RoomPPE used/ preferredSample collection/ reception roomLab coat, gloves Smear microscopy section/ room/ Designated Microscopy Centre (DMC)Lab coat, glovesCartridge-based Nucleic Acid Amplification Test (CBNAAT) sample processing sectionLab coat, gloves, Surgical maskSample opening area(in a higher laboratory) Surgical gown, gloves and N95 respirator Media preparation room Designated lab coat, gloves, hair cover, shoe covers/ closed-toe shoes Culture reading roomLab coat, gloves, N95 respiratorLine Probe Assay (LPA) clean roomsDesignated lab coat, gloves, hair cover, shoe covers/ closed-toe shoesWalk-in cold roomLab coat, insulating gloves, shoe covers/ closed-toe shoesWalk-in incubatorLab coat, respirator and gloves, shoe covers/ closed-toe shoesCorridor inside the labLab coat, shoe cover/ closed-toe shoesDeep freezersLab coat, cryo glovesDisinfection, washing and sterilisation roomLab coat, gloves (heavy duty), insulating gloves, closed-toe shoesResources
- National Guidelines for Infection Prevention and Control in Healthcare Facilities, 2020, MoHFW, GoI.
Resources
Use of a PPE in a DMC
ContentThe use of appropriate Personal Protective Equipment (PPE) in a TB laboratory is determined by risk assessment (according to the procedure and suspected pathogen).
Designated Microscopy Centres (DMCs) are low-risk TB laboratories, hence PPE should be used as follows:
- Laboratory coats should be worn at all times by the Laboratory Technician (LT) while working in the laboratory.
- Gloves and long-sleeved laboratory coats should be used during sample collection, opening sample transport boxes, handling leaky specimen containers, smear preparation and staining smears.
- Masks are not required for use during the preparation of sputum smears in well-ventilated areas.
- LTs and support staff handling biological waste should wear gloves.
- Patients that visit DMC to provide sputum samples should be advised to wear masks.
It is advised that the laboratory should maintain adequate ventilation by keeping the windows open all the time or installing exhaust for the personal protection of the laboratory staff.
Resources
- Guidelines on Airborne Infection Control in Healthcare and Other Settings, MoHFW, 2010.
- Infection Prevention and Control of Epidemic- and Pandemic-Prone Acute Respiratory Infections in Health Care, WHO, 2014.
- Training Modules (1-4) for Programme Managers and Medical Officers, NTEP, 2020.
Assessment
Question
Answer 1
Answer 2
Answer 3
Answer 4
Correct answer
Correct explanation
Page id
Part of Pre-test
Part of Post-test
LTs and support staff handling biological waste should not wear gloves.
True
False
2
LTs and support staff handling biological waste should wear gloves.
Yes Yes Laboratory Gowns for Use by Lab Personnel
ContentLaboratory Gowns (Figure 1)
- Protect the skin and clothing from large droplets of infectious or hazardous materials that may be splattered in the laboratory.
- Gowns must be worn for specimen processing, tuberculosis (TB) culture and drug sensitivity testing (DST).
- The gown must have a solid front and close and tie in the back.
- The gown must have long-sleeves and cuffs.
- For maximum protection, gloves must be pulled over the cuff.
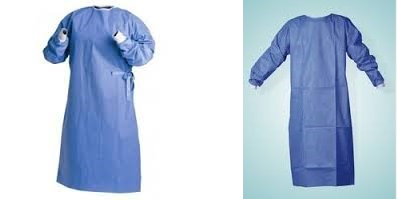
Figure 1: Laboratory Gowns
Laboratory Coats (Apron) (Figure 2)
- Lab coats must be worn when working on specimens and acid-fast bacilli (AFB) smears and not during TB culture work.
- Lab coats must be made from washable and autoclavable cloth or disposable materials.
- It must be closed up in the front (with snaps, buttons or velcro) and must have long sleeves.
- It must be buttoned till the top at all times in the lab.

Figure 2: Laboratory Coat
Do’s and Don’ts for Laboratory Gowns and Coats
- The laboratory gown must be laundered once a week and immediately after being overtly contaminated.
- If staff is using a reusable gown, it must be laundered and sterilized as required before reuse.
- Used gowns must be stored in separate cupboards or lockers.
- Hang the gown on designated hooks in the lab.
- Lab gowns must not be worn outside the laboratory, e.g., in communal areas, toilets, offices, etc.
- Staff must wear appropriately sized gowns and coats.
- Lab coats must not be taken home for washing. Laboratory personnel in-charge must arrange for cleaning from the worksite only. Before laundering, the gowns and lab coats must be disinfected or autoclaved.
Resources
Kindly provide your valuable feedback on the page to the link provided HERE
Donning and Doffing of PPE
ContentSequence of Donning of Personal Protective Equipment (PPE): (How to put on PPE)
- Footwear
- Gown
- N-95 respirator
- Goggles and face shield
- Gloves
Donning must be done before entering the patient/ laboratory area.
Sequence of Doffing of PPE: (How to safely remove PPE)
- Gown and gloves
- Footwear
- Goggles and face shield
- N-95 respirator
- Wash hands or use an alcohol-based hand sanitizer immediately after removing all PPE.
Where to remove PPE?
- PPE must be removed at doorway, before leaving the patient room or in the anteroom.
- Staff must remove respirator outside the room, after the door has been closed.
Four Key Points to Remember about PPE Use
- Staff must don the PPE before any contact with the patient, generally before entering the room.
- After wearing the PPE on, staff must remain careful to prevent spreading contamination.
- After completing the tasks, staff must remove the PPE carefully and discard it in the receptacles provided.
- After removing the PPE, immediately hand hygiene must be performed before going on to the next patient.
Click the video below to see the donning and doffing of PPE.
Resources
- Manual for Donning and Doffing of PPE by Center for Disease Control and Prevention (CDC).
- Steps to put on Personal Protective Equipment (PPE), WHO Poster.
Kindly provide your valuable feedback on the page to the link provided HERE
N95 Respirators for TB Lab Personnel
ContentN95 respirators are Personal Protective Equipment (PPE) used as a biosafety measure in clinical and laboratory settings.
N95 Respirators
- N95 filtering facepiece respirators are air-purifying respirators.
- Certified to have a filter efficiency level of 95% or greater against particulate aerosols free of oil and 0.3 microns in size.
- N95 (United States Standard NIOSH N95) or program-specific guidelines should be followed in the selection of these respirators.

Figure: N95 Respirators
Use of N95 Respirators in TB Laboratories
- Not required in low- and moderate-risk TB laboratories but are required in high-risk TB laboratories
- Must be available in laboratories where culture manipulations are performed
- Should be included as part of a laboratory’s spill clean-up kit
- Should never be used as a substitute for a properly maintained and functioning Biosafety Cabinet (BSC) and other PPE
Approval Required for N95 Use
Personnel who are required to wear respirators, shall be approved for N95 use after completing the following:
- Medical Evaluation/ Clearance: To determine if users are physically fit to wear a respirator.
- Training: To ensure users are familiar with N95 respirators, their proper use and protective limitations.
- Fit-testing: To determine which respirator model/ size provides the proper fit for the user. Such a fit-test is required on an annual basis and when a different model is being used or there are changes in facial characteristics.
Table: Showing the difference between user seal check and fit-test
USER SEAL CHECK
FIT-TEST
Should be conducted each time a respirator is put on, to determine if it is properly sealed to the face.
- Evaluation of how a respirator fits, conducted by trained personnel. (Includes the use of a scented solution and the determination of whether the employee can detect the odour/ taste).
- Should be conducted prior to the use of a respirator and annually thereafter OR when a new respirator is being introduced.
Limitations of N95 Respirators
- N95 respirators ONLY filter out particulate contaminants. N95 respirators do not protect from chemical vapours/ gases, high-risk exposures such as those created by aerosol-generating procedures (i.e., bronchoscopy, autopsy) and asbestos handling.
- N95 respirators are generally single-use disposable. Considering the funding constraints for TB labs, the availability of N95 can pose a challenge.
Comparison between the Surgical Mask and N95 Respirators
- The purpose of a surgical mask is to protect the environment or the community from the wearer of the mask. It is usually worn by a patient infected with TB or other infectious diseases to protect others.
- Unlike the N-95 respirator, a surgical mask offers less protection to the wearer from aerosolized TB and is unable to form a tight seal; thus aerosols are able to come in through the gaps.
Disposal of N95 Respirators
- TB lab personnel must remove the mask using the appropriate technique (i.e., must not touch the front but remove the lace from behind), only after coming out of the laboratory.
- Staff must clean their hands by using an alcohol-based hand rub or soap and water, after removal or whenever inadvertently touching a used mask.
- N-95 mask must be discarded and collected in separate 'yellow colour-coded plastic bags' (suitable for biomedical waste collection).
Resources
- National Guidelines for Infection Prevention and Control in Healthcare Facilities, 2020. Ministry of Health and Family Welfare, Government of India.
- Importance of a User Seal Check, Manual from 3M Science.
- Frequently Asked Questions about Respiratory Protection by Center for Disease Control and Prevention (CDC).
Kindly provide your valuable feedback on the page to the link provided HERE
Gloves for TB Lab Personnel
Content- Gloves are made for protecting the hands of health professionals from contaminated and infectious surfaces.
- Lab staff must wear gloves for all the procedures that involve direct or accidental contact with infectious material.
- Gloves are made for single-use (disposable gloves) and should not be re-used (see Figure 1)
- Gloves are made from vinyl, latex or nitrile.
- For the staff who are allergic to latex and when performing PCR, nitrile gloves should be available for use.
Figure 1: Disposable Gloves
Do’s when using gloves
- Staff must select and use the right kind of glove for the job they are going to perform.
- Always use the correct size of gloves. Staff regularly need to check the fitness and size suitable for them.
- Gloves must be resistant to the chemical used during the procedure.
- Staff must inspect their gloves before using them.
- Before wearing gloves, staff must remove any rings, watches, or bracelets that might cut or tear the gloves.
- If gloves are torn during a procedure, replace them immediately (Figure 2).
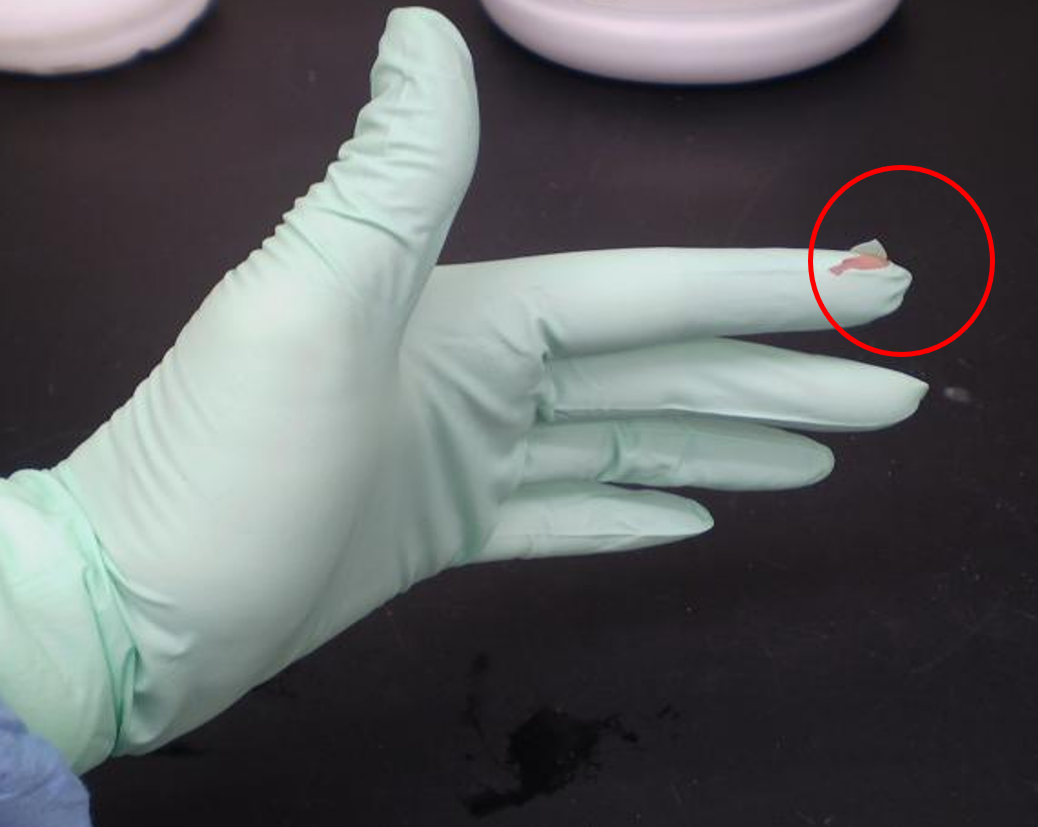
Figure 2: Torn gloves need immediate replacement
- Staff must wear double gloves when working with potentially hazardous materials in the biosafety cabinet.
- Staff must pull the gloves over the cuff of the lab gown for maximum protection.
- Staff must change the gloves:
- At the end of the task
- If gloves are soiled/punctured
- Soiled gloves must be discarded in the bag provided for waste disposal.
- Gloves guard against infection through cuts and abrasions on the hands. Cuts and abrasions must be covered with a sticking plaster and/or suitable barrier dressing at all times while in the laboratory
- Cryo gloves should be used while handling deep freezers and cotton gloves should be use while handling the autoclave
Don’ts when using gloves
- Contaminated gloves must not be used to handle or to operate equipment (e.g., microscope or telephone), that would otherwise never become contaminated.
- Staff must never wear gloves outside the laboratory.
- After wearing gloves, staff must avoid/limit touching any surface
Resources
Kindly provide your valuable feedback on the page to the link provided HERE
Fullscreen