-
STLS: General concepts in specimen collection & transportation
FullscreenNeed for Specimen Collection and Transportation [SCT]
ContentThe National TB Elimination Programme (NTEP) has strengthened sputum collection and transport for laboratory testing by building capacity for decentralised collection.
- The provision for sputum collection and transport is used to establish linkages for giving diagnostic access to patients who cannot reach the health facilities.
- To increase access and coverage of services, designated sputum collection centres are also established for collecting and transporting sputum to the nearby laboratory.
Presumptive TB patients attending Peripheral Health Institutions (PHIs) other than Designated Microscopic Centres (DMCs) are either referred to the nearest DMC for sputum examination or their sputum specimens are collected and transported to the DMC as per guidelines.
- The patient is given these options as per their convenience to minimise the possible delay in diagnosis and initiation of treatment or avoid repeated visits by the patient.
- In case the patient is not able to travel to the DMC, then the spot sample is collected at the nearest health facility/ sputum collection centre/ sputum collection booths and transported to the DMC.
The need for sample collection can be categorized broadly into two categories:
1. When samples are sent to the DMC
- Some PHI/ sub-centres/ health and wellness centres function as sample collection centres.
- Sputum collected from referring health facilities needs to be transported to the nearest DMC.
2. When DMC has to collect and transport samples for testing/ follow-up/ resistance testing to higher laboratories
- If the Nucleic Acid Amplification Testing (NAAT) facility is not available at the health facility, the DMC may also need to collect and send the sample to the nearest linked facility for NAAT testing.
- If NAAT is available at DMC and Mycobacterium tuberculosis (MTB) is detected, the second sample needs to be transported to the Culture and Drug Susceptibility Testing (C&DST) lab. If the NAAT result suggests rifampicin-sensitive, a second sample is sent for First-line Line Probe Assay (FL-LPA) to look for H-mono/ poly resistance.
- Extrapulmonary samples have to be appropriately collected at the PHI/HF and transported for testing to NAAT/ culture facilities.
Resources
Assessment
Question
Answer 1
Answer 2
Answer 3
Answer 4
Correct answer
Correct explanation
Page id
Part of Pre-test
Part of Post-test
Specimen collection and transportation system minimises patient inconveniences and diagnostic delays.
True
False
1
Specimen collection and transportation system minimises patient inconveniences and diagnostic delays.
Yes Yes Process of SCT
Content- Good quality sputum collection is of paramount importance in tuberculosis diagnosis.
- Once a person is identified as presumptive TB, s/he is referred to the Designated Microscopy Centre (DMC) for sputum collection.
- For TB diagnosis two sputum samples are collected - one is the supervised ‘spot’ sample collected at the DMC (labelled Specimen A) and the other is the early morning sample collected by patient themselves at his/her home (labelled Specimen B).
- If the patient is coming from a long distance or s/he is unlikely to return to give the second specimen, two spot specimens may be collected with a gap of at least one hour.

Figure: Flowchart for Sputum Collection and Transport
Sputum Collection
- The (NTEP) request form required for the biological specimen examination need to be filled.
- The Lab Technician (LT) should instruct the patient to thoroughly rinse the mouth with clean water and demonstrate to inhale deeply 2-3 times and cough out the sputum from the depth of the chest into a sterile 50 ml sputum container, in a well-ventilated space.
- After collecting the sputum, close the lid of the containers and wipe the surface of the tube with 5% phenol to disinfect and allow it to air dry.
- Label the tubes with patient details, date and time of collection, specimen identification, lab no. using a permanent marker.
Sputum Transport
- The sputum collected should be transported immediately to the Nucleic Acid Amplification Testing (NAAT)/ Culture and Drug Susceptibility Testing (C&DST) laboratory. In case of any unavoidable delays, the sample should be refrigerated.
- The programme mandates triple layer packaging for the transport of the sputum specimens.
- Firstly, seal the joint between the cap and neck of the sputum containers with a parafilm strip (primary receptacle package).
- Wrap the sputum containers individually in absorbent cotton, place them in a zip lock pouch and secure them with a rubber band (secondary receptacle package).
- Fold and place the NTEP request form in another zip lock pouch.
- Place the zip lock pouch with sputum containers in a thermocol box along with two pre-frozen coolant gel packs and the zip lock pouch with the NTEP request form is placed on top.
- The dimensions of the thermocol box used for sputum transport are: thickness - 2.5 cm; Outer dimensions: length - 18.5 cm, breadth - 13 cm, height - 12 cm (without lid), height -14 cm (with lid); Inner dimensions: length - 14.5 cm, breadth - 8 cm, height - 12 cm (without lid), height - 13 cm (with inner part of lid).
- The coolant gel packs should be conditioned in the deep freezer in a temperature between -20 to -15o C for a minimum 48 hours to a maximum 72 hours before use so that they can maintain a temperature between 12-20o C for up to approximately 48 hours in tightly packed thermocol boxes while the average outside temperature is 35o C.
- Seal the thermocol box with duct tape and affix ‘To’ and ‘From’ address, biohazard sticker on the box (tertiary receptacle package).
- Weight of the fully packed consignment box should be up to 400 grams and the thermocol boxes and gel packs should not be reused.
- Transport the box through NTEP identified courier/ speed post service.
Resources
- Training Module (1-4) for Programme Managers and Medical Officers, NTEP, MoHFW, 2020.
- Guidelines for Programmatic Management of Drug-resistant TB in India, 2021.
- Module for Laboratory Technician, CTD, MoHFW, India, 2005.
Assessment
Question Answer 1 Answer 2 Answer 3 Answer 4 Correct answer Correct explanation Page id Part of Pre-test Part of Post-test After collecting the specimen, the falcon tubes should be wiped and disinfected with which solution? 5% Iodine 5% Glycerine 5% Phenol 5% Sodium 3 After collecting the specimen, the falcon tubes should be wiped and disinfected with 5% phenol solution. Yes Yes NTEP mandates triple layer packaging for the transport of the sputum specimens
True False 1 Triple layer packaging prevents spills and leakages during transportation of sample. Yes Yes Modes of Transportation in SCT
ContentAll efforts must be made to have decentralised local arrangements for transporting the specimens to the TB detection centre (TDC). If a proper transport mechanism for collected specimen is in place, it spares the patients from travelling to the laboratory.
The sputum sample is packaged in triple layers in such a manner that it arrives at the destination in good condition and presents no hazard to the transporter.
Transporter/ personnel transporting the sample should be sensitized by the National TB Elimination Programme (NTEP) staff prior to engagement.
- Sensitisation would be provided on Symptoms of TB disease and its transmission, precautions to be taken to prevent exposure, hand hygiene requirements and spill management.
The different modes of sample transport include:
1. Post: Postal department services available pan-district can be engaged to transport sputum samples.
2. Courier: Local logistics courier companies can also be identified and hired to transport samples.
3. Volunteers/ human carriers: Community volunteers/members of NGOs can be trained as human carriers to collect and transport samples.
District TB Centre or Medical Officer TB Control (MO-TC) should ensure feasibility and financial measures required for .such arrangements for sputum transport.
Systems can be established for transportation of various biological samples (not only TB) from referring centre/peripheral centre to laboratories in a hub and spoke model in a integrated manner.
Resources
- Specimen Transportation - A How-to Guide.
- Health and Safety Guidelines for Staff/ Workers involved in Sputum Transportation, CTD.
Assessment
Question
Answer 1
Answer 2
Answer 3
Answer 4
Correct answer
Correct explanation
Page id
Part of Pre-test
Part of Post-test
Sputum can be transported through post/ courier/ human carriers.
True
False
1
Sputum can be transported through post/ courier/ human carriers.
Yes Yes Specimen Collection and Transportation to a DMC
ContentSputum collection centres collect, package and then transport samples to nearby TB diagnostic centres/ Designated Microscopy Centre (DMC).
Sputum is collected and packaged utilizing the triple-layer packing as per National TB Elimination Programme (NTEP) Guidelines.
ImageThe Multi-purpose Health Worker (MPHW) or the Laboratory Technician (LT) at the sputum collection centre are responsible for collecting the right specimen, enrolling the presumptive TB case in Niskshay, generating Nikshay ID and testing ID for the requested test.
Sputum is transported in the sample transport box to the nearest laboratory along with the completely and correctly filled laboratory request form (along with Test ID generated through Nkshay). Sputum can be transported utilizing local volunteers, courier services, etc.
Ideally the sputum needs to be transported without delay. In case, the delay is expected, then the cold chain also needs to be maintained.
Resources
- Training Modules (1-4) for Programme Managers and Medical Officers, NTEP, 2020.
- Operational Guidelines for TB Services at Ayushman Bharat Health and Wellness Centres, 2020.
Assessment
Question Answer 1 Answer 2 Answer 3 Answer 4 Correct answer Correct explanation Page id Part of Pre-test Part of Post-test LT at sputum collection centres enrols the patient and generates a test request on Nikshay. True False 1 LT at sputum collection centres enrols the patient and generates a test request on Nikshay. Yes Yes Cold Chain Requirement for the Transport of TB Diagnostic Specimens
ContentA cold chain is a system of transporting and storing TB specimens at optimum temperature while being transported from the peripheral health institutions to the diagnostic labs to reduce the growth of contaminating endogenous respiratory organisms.
Cold chain requirements for transportation of TB diagnostic specimens are (Figure 1):
- A thick thermocol box (one-time use box), which has a thickness of about 2.5 cm. Outer dimensions of the box - Length: 18.5 cm, Breadth: 13 cm, Height: 12 cm. Inner dimensions of the box - Length: 14.5 cm, Breadth: 8 cm, Height: 10 cm.
- Two gel packs to maintain a temperature between 12-20°C for up to approximately 48 hours in tightly packed thermocol boxes (average outside temperature 35°C). Gel packs to be conditioned in the deep freezer (temperature between -20 to -15°C) for a minimum of 48-72 hours before use.

Figure 1: Technical specifications of transport box for sputum specimen transportation in cold chain
Specimen Transport Steps - Cold Chain (Figure 2)
- Place the gel pack into the thermocol box.
- Place the sample tubes (in zip-lock pouches) on the frozen gel packs.
- Keep the pouch containing the Test Request form on top before placing another gel pack on top.
- Close the lid of the box and wrap tightly with brown duct tape to maintain the cold chain.

Figure 2: Steps for specimen transportation in cold chain
Resources
Kindly provide your valuable feedback on the page to the link provided HERE
-
STLS: Packaging & dispatching sample to a C&DST lab
FullscreenRequirements for Packaging a biological Specimen
ContentPeripheral Laboratories in the NTEP need to send biological samples (such as sputum) to nearby Culture and Drug Susceptibility Testing (CDST) laboratories for advanced testing (eg Drug Resistance Testing). The samples need to be safely packaged and transported such that there is no spillage or contamination.
The items required for safe packaging biological specimens are:
- Falcon tubes
- Three-layer packing materials like thermocol box
- Ice gel pack (pre-frozen at -20oC for 48 hours)
- Request for CDST forms
- Polythene bags
- Tissue paper roll for absorbent packing
- Parafilm tapes
- Brown tape for packing the thermocol box
- Permanent marker pen
- Labels with 'To' and 'From' address and blank labels for sample details
- Biohazard sticker
- Scissors
- Spirit swab
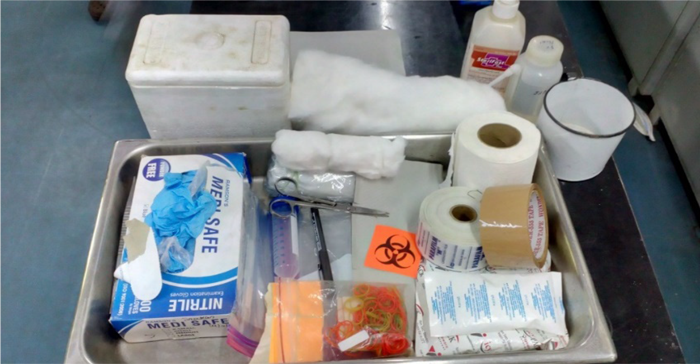
Figure: Items needed for packaging of biological specimens for CDST laboratory; Source: Guidelines for Programmatic Management of Drug Resistant TB in India, 2021
Video fileResources
Specimen Carriers
ContentTechnical specifications for TB diagnosis specimen carriers are as follows:
Thermocol Box:
- Thickness of box - 2.5 cm
- Outer dimensions: Length - 18.5 cm, breadth - 13 cm, height - 12 cm (without lid), height - 14 cm (with lid); Inner dimensions: Length - 14.5 cm, breadth - 8 cm, height - 12 cm (without lid), height - 13 cm (with inner part of lid).
Gel Pack:
- Number of gel packs required: 2
- Weight of fully packed consignment box: 400 grams
- Gel packs maintain a temperature between 12-20ºC for up to approximately 48 hours in tightly packed thermocol boxes (average outside temperature 35ºC)
- Conditioning in the deep freezer (temperature between -20 to -15ºC) for a minimum 48 hours to a maximum 72 hours before use, is required.
This is a one-time use carrier since the thermocol boxes and the gel packs are not reused.

Figure: TB Diagnostic Specimen Carrier - Thermocol Box with Gel Packs; Source: NTEP Guidelines for Programmatic Management of Drug Resistant TB in India, 2021
Resources
- Training Module (1-4) for Program Managers and Medical Officer, NTEP, MoHFW, 2020.
- Guidelines for Programmatic Management of Drug Resistant TB in India, 2021.
Kindly provide your valuable feedback on the page to the link provided HERE
SOP for Packaging Specimens during the Transportation of Biological Specimens for TB Diagnosis
ContentStandard Operating Procedure (SOP) for Packaging Specimen during the transportation of biological specimens for TB diagnosis, also known as Triple Layer Packaging, is as follows:
The Lab Technicians (LTs) at the Designated Microscopy Centres (DMCs) should be trained to carefully pack the sputum samples in the cold box to avoid spillage of the samples. Before packing, personal protection measures such as wearing hand gloves (double gloves preferred), goggles and masks are to be followed by the LTs to prevent contracting the infection.
Table: Steps in Standard Operating Procedure (SOP) for Packaging Specimen during Transportation for TB Diagnosis
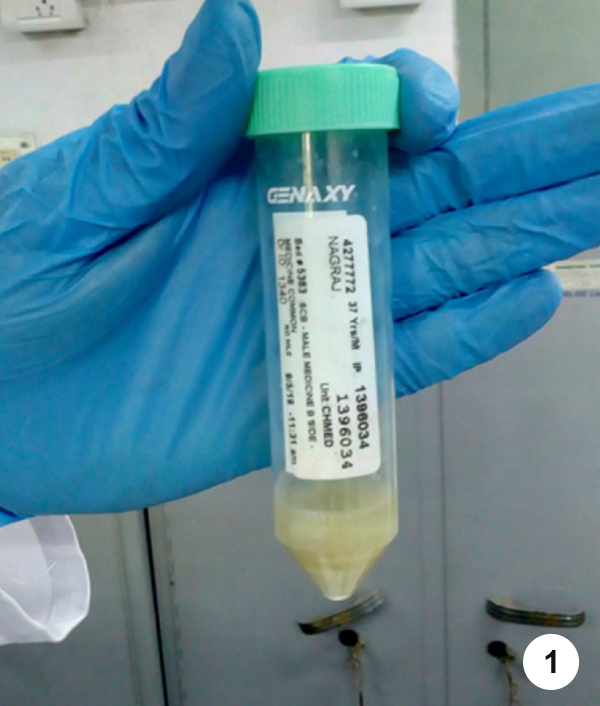
- Step 1. Make sure that the specimen collection tube is tightly closed after the sample has been collected from the patient.

- Step 2. Wipe the outer surface of the 50 ml conical tube with 5% phenol followed by absorbent tissues and allow it to air dry.

- Step 3. Write the patient details on the opaque area (white area) of the specimen collection tube using a permanent marker pen, clearly in capital letters.
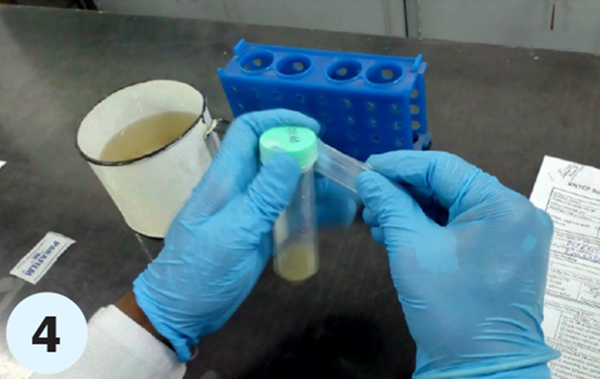
- Step 4. Cut the parafilm strip and wrap one of the strips at the joint between the cap and the neck of the specimen collection tube such that a secured seal is formed. (Primary receptacle/ package

- Step 5. Open the absorbent cotton roll and spread it out on the workbench; separate the cotton into two equal layers. Roll the specimen collection tube containing the sample tightly in the absorbent cotton such that the tube is covered completely.
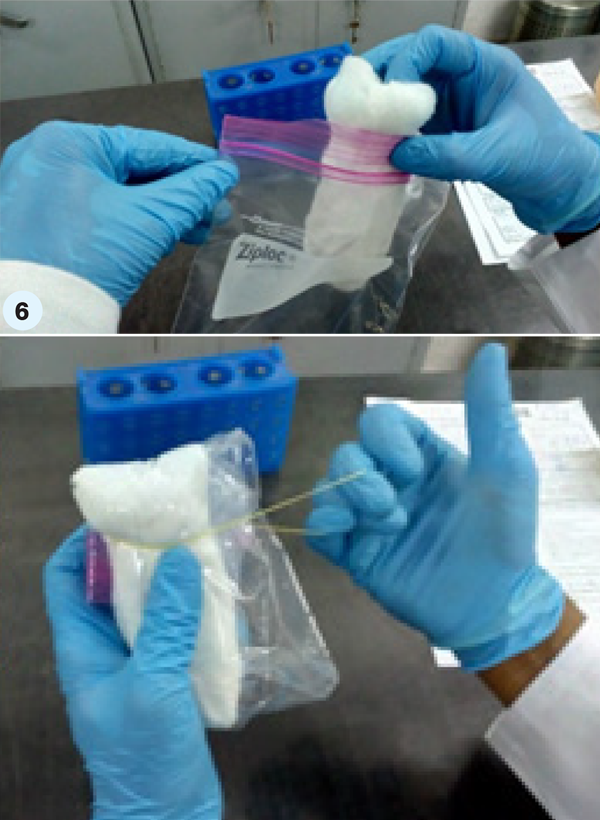
- Step 6. Put this roll containing the specimen collection tube into the ziplock pouch. Roll the whole into a tight bundle, ensuring that there is no air in the pouch. This bundle should be secured with rubber bands. (Secondary receptacle/ package)


- Step 7. Repeat steps 5–7 for the second sample of the patient.

- Step 8. Insert the Test Request form printed from Nikshay into the ziplock pouch after ensuring that the details on the form and the sample tubes match, with the writing facing outside (details visible through the package). Seal the ziplock on the pouch.

- Step 9. Place the cooled gel packs into the thermocol box, place the sample tubes packed in ziplock pouches on the frozen gel packs (frozen for 48 hours at -40°C) and also keep the pouch containing the Test Request form printed from Nikshay on top. Stick the BIOHAZARD sign over the lid and “To and From” stickers on the exterior of the thermocol box or box used to pack the specimen. Close the lid of the box and wrap it tightly with brown duct tape. (Tertiary receptacle/ package)

- Step 10. Complete the ‘From’ and ‘To’ addresses on the stickers, using a permanent marker pen.
The LT of the DMC should promptly inform the sample transport agency like a courier/ speed post service, or a human carrier to collect and transport the samples.
Video fileResources
- Training Module (1-4) for Program Managers and Medical Officers, NTEP, MoHFW, 2020.
- Guidelines for Programmatic Management of Drug-resistant TB in India, 2021.
Kindly provide your valuable feedback on the page to the link provided HERE
Technical Specifications for Labelling Specimen Transport Carriers
ContentThese are the technical specifications for labelling specimen transport carriers:
- Specimen containers need to be labelled legibly with details such as the patients’ name, date and time of specimen collection, TB detection centre/ District Tuberculosis Centre (DTC), lab no., specimen A or B.


Figure: Details to be filled on the specimen containers

- Dispatch list with details of each specimen transported and the request form for examination of biological specimen for each specimen should be put in an envelope and attached to the outside box.
- As per the national guidelines for biomedical waste management, the containers used for transporting specimen samples to the National TB Elimination Programme (NTEP) - certified laboratory should be labelled with a “BIOHAZARD” sticker.

- Other than the Biohazard sticker it is mandatory to add 'To' and 'From' stickers on the specimen transportation carrier and fill in the necessary details.
- Specimen transport carriers should be labelled legibly with all the necessary details as listed above.
- A specimen may be rejected at the receiving laboratory if the specimen transport carriers are unlabelled or mislabelled.
Resources
Kindly provide your valuable feedback on the page to the link provided HERE
Dispatching the sample to a C&DST Lab
ContentFor presumptive Drug-resistant TB (DR-TB) patients’, the health facility staff arranges for specimen collection from patient, packs samples as per the Standard Operating Procedure (SOP) for triple layer packaging and dispatches it for transportation in cool chain to the linked Culture and Drug Susceptibility Testing (C&DST) laboratory.
All necessary materials for specimen collection and modality for transportation need to be made available/ arranged at the Designated Microscopy Centre (DMC)/ Peripheral Health Institute (PHI) by the District TB Officer (DTO).
Steps in sample dispatch include:
- Add test details in Nikshay (Figure) to generate test requests (Test ID) for the patient’s episode ID in Nikshay.
- This will enable instant online intimation about the upcoming specimen to the C&DST laboratory.
- Complete test request form for biological specimen by adding:
- Patient information
- Details on name and type of referring facility
- Health establishment ID
- Reason for testing and test requested
- Patient ID and Test ID
- Put the appropriate address of receiving C&DST laboratory and address of health facility form where samples are dispatched on the transportation box.
- Lab Technician (LT) of the health facility should promptly inform the transport agency (courier/ speed post service) or human volunteers to collect and transport the samples.

Figure: Adding Test Details in Nikshay for Diagnosis of DR-TB; Source: Nikshay Diagnostics Training Content.
Resources
- Training Modules (1-4) for Programme Managers and Medical Officers, NTEP, 2020.
- Guidelines for PMDT in India, 2021.
- Nikshay Zendesk, Nikshay Knowledge Base, Diagnostics.
Assessment
Question
Answer 1
Answer 2
Answer 3
Answer 4
Correct answer
Correct explanation
Page id
Part of Pre-test
Part of Post-test
Test details are added in Nikshay to generate test requests (Test ID) for the patient’s episode ID in Nikshay.
True
False
1
Test details are added in Nikshay to generate test requests (Test ID) for the patient’s episode ID in Nikshay.
Yes
Yes
- Add test details in Nikshay (Figure) to generate test requests (Test ID) for the patient’s episode ID in Nikshay.
Fullscreen

