National TB Elimination Program [NTEP]
Content- The National Tuberculosis Elimination Program (NTEP) is the public health initiative of the Government of India that organizes the country’s Tuberculosis Elimination efforts.
- NTEP is a centrally sponsored scheme being implemented under the aegis of the National Health Mission with resources sharing between the State Governments and the Central Government.
- The program provides various free of cost, quality tuberculosis diagnosis and treatment services across the country.
Image
Resources
- Training Modules (1-4) for Programme Managers and Medical Officers; New Delhi, India: Central TB Division, MoHFW, Government of India, July 2020
- India TB Report 2021
Kindly provide your valuable feedback on the page to the link provided HERE
Tuberculosis Unit [TU]
ContentTuberculosis (TB) unit (TU) is the sub-district level supervisory unit of National TB Elimination Program with the following organogram:
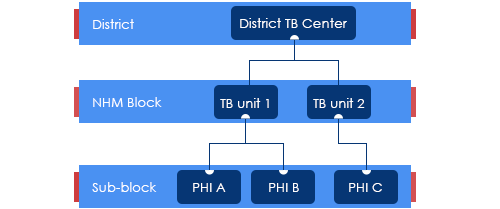
Figure: Organogram of a TB Unit
(PHI: Peripheral Health Institution)
TUs are based mainly on National Health Mission (NHM) health blocks with the aim of aligning with the NHM Block Programme Management Unit (BPMU) for optimum resource utilization and appropriate monitoring.
The TUs have been created based on a population of 1 per 2,00,000 (range 1.5 – 2.5 lakh) for rural and urban populations and 1 per 1,00,000 (0.75 – 1.25 lakh) population in hilly/tribal/difficult areas.
The TU consists of a designated Medical Officer-Tuberculosis Control (MO-TC), as well as one full-time supervisory staff - Senior Treatment Supervisor (STS). However, one Senior TB Laboratory Supervisor (STLS) will be there in every 5 lakh population (one per 2.5 lakh population for tribal/hilly/difficult areas), mostly covering 2-3 TUs.
TB Unit manages the provision of TB services (Diagnosis, Treatment, Prevention, etc.) and programme management in the assigned geographical area.
Resources
Stages in TB Patient's Lifecycle
ContentThose who are suspected of having TB disease are first screened for symptoms like cough and fever for more than 2 weeks, blood stained sputum and weight-loss. If found positive on screening, then TB patients are referred for testing to the nearest health facility. If diagnosed with TB, then they are subsequently initiated on treatment. The TB patients initiated on treatment are regularly monitored with the help of field staff or digital interventions like 99DOTS and MERM (Medication Event Reminder Monitor) technology. NTEP staff also ensures that the TB patients are regularly followed up on monthly basis till their treatment completion.

Figure: Patient Flow
Kindly provide your valuable feedback on the page to the link provided HERE
Categorization of TB Treatment Regimen
ContentDaily Regimen is prescribed for TB patients, where patients need to consume the medicine daily.
Daily Regimen comprises of the first line Anti TB drugs, based on
- Age: Adult/Paediatric
- Weight of the patient: Weight Bands
Age: Based on the age, patients are categorized into
- Adults: Patient's age should be 19 years or more.
- Paediatrics: Patient's age up to 18 years and weight less than 39 Kgs
Weight Bands:
- Treatment dosage is based on the TB patient’s weight.
- A weight band category is defined for Adult and Paediatric patients separately and medicines are issued based on that weight category.
TB Case classification in NTEP
ContentTB cases are generally classified on the basis of previous history of TB treatment into New and previously treated cases.
New case - A TB patient who has never had treatment for TB or has taken anti-TB drugs for less than one month is considered as a new case.
Previously treated patients have received 1 month or more of anti-TB drugs in the past. They could be further classified as:
- Recurrent TB case - A TB patient previously declared as successfully treated (cured/treatment completed) and is subsequently found to be microbiologically confirmed TB case is a recurrent TB case.
- Treatment After failure patients are those who have previously been treated for TB and whose treatment failed at the end of their most recent course of treatment.
- Treatment after loss to follow-up - A TB patient previously treated for TB for 1 month or more and was declared lost to follow-up in their most recent course of treatment and subsequently found microbiologically confirmed TB case
- Other previously treated patients are those who have previously been treated for TB but whose outcome after their most recent course of treatment is unknown or undocumented.
Resources:
Kindly provide your valuable feedback on the page to the link provided HERE
Patient interaction with TB Care Ecosystem
ContentHealth Volunteers/ Treatment Supporters are often the regular point of contact for a TB patient in the community. They support the TB patient during the entire episode of TB and ensure complete diagnosis and treatment. The next points of contact are with the MPHWs who periodically visit the patients to ensure specific delivery of services.
The Peripheral HeaIth Institution (PHI) is the nearest accessible health facility where the patient can access a physician/ doctor for diagnosis and treatment services. These are often in the form of a Primary Health Centre, but can also be higher level institutions such as medical colleges and private health facilities that are most accessible to/ preferred by the patient. The PHI may also host a drug store/ pharmacy from where the patient's medicines would be dispensed.
Other health facilities with diagnostic services such as DMCs, NAAT Sites and C&DST Labs may be accessed by the patient or by their biological specimen being collected and transported to the corresponding laboratory. Other higher order health institutions such as DRTB Centres may also be accessed by the patient on referral.
The District TB Centre, TB Unit and its staff provide programmatic support and supervision indirectly through the PHI. At times the National Call Centre may contact the patient for providing specific information, or for collecting feedback on quality of service delivery.

Figure: Stakeholders interacting with HVs
Resources:
Kindly provide your valuable feedback on the page to the link provided HERE
Role of Health Volunteers
ContentHealth Volunteers
- are members of the communities where they work,
- are supported by the health system but not necessarily a part of its organization,
- and have shorter training than professional workers”

Figure: Role of Health Volunteers
Resources:
Kindly provide your valuable feedback on the page to the link provided HERE
Fullscreen