Presumptive TB
ContentPresumptive TB case refers to a patient who presents with symptoms or signs suggestive of TB disease (previously known as a TB suspect) and where further diagnostic workup including bacteriological investigation is required.
Presumptive TB can be categorized into
-
Presumptive Pulmonary TB (P TB) - Symptoms are directly related to lungs (Cough, hemoptysis)
-
Presumptive Extra Pulmonary TB (EP TB) - Symptoms/ signs are specific to an extra pulmonary site (example: Lymph node swelling)
-
Presumptive Pediatric TB - Symptoms of TB in young children are more difficult to identify and can be more general (fever, weight loss)
Resources:
- Technical and Operational Guidelines for TB Control in India 2016
- Definitions and reporting framework for tuberculosis
Kindly provide your valuable feedback on the page to the link provided HERE
-
Principles of TB Diagnosis under NTEP
ContentThe National TB Elimination Program (NTEP), promotes the following principles to diagnose TB:
- Try to establish the microbiological confirmation for all cases
- Use rapid molecular diagnostics upfront wherever possible for diagnosis of TB and early identification of resistance to treating drugs.
- Focus more on quality sample collection and timely transportation for a better microbiological confirmation
Microbiological Confirmation for All Cases
Microbiologically confirmed TB refers to a presumptive TB case from whom a biological specimen is positive for acid fast bacilli smear microscopy, or positive for Mycobacterium tuberculosis on culture, or positive for TB through Rapid Diagnostic molecular tests - Nucleic Acid Amplification Test (NAAT) and Line Probe Assay (LPA). Establishing microbiological confirmation is key for all TB cases. Clinically diagnosing TB should be limited only to very few patients where, in-spite of high suspicion, microbiological confirmation could not be established, even after all possible efforts. The entire diagnostic algorithm puts utmost efforts to establish the microbiological evidence in a case of TB.
Upfront Rapid Molecular Diagnostics
Knowing the drug resistance pattern at the earliest is key for success of the treatment. Hence, the current policy highlights the importance of using molecular diagnostic test upfront wherever possible.
Complete diagnosis of TB is achieved by:
- Offering NAAT (CBNAAT/ Truenat) to all notified new patients and to test for resistance to Rifampicin. This is termed as Universal Drug Sensitivity Test (DST) for Rifampicin. Efforts are being made to collect specimen from all TB patients for NAAT at baseline.
- Testing individuals belonging to key population groups (clinically, socially vulnerable), those with extra pulmonary TB, people living with HIV and paediatric patients (after X-ray screening). They are directly referred for TB testing by NAAT
- For upfront NAAT, one specimen is tested using NAAT and if TB is detected, the other sample is used for further cascade testing by LPA and liquid culture
Quality Sample Collection and Transport
For TB diagnosis, it is essential that a good sputum sample is collected. A good specimen consists of recently discharged material from the bronchial tree with minimum amount of oral or nasopharyngeal material, presence of mucoid or mucopurulent material and should be 2-5 ml in volume. The specimen is collected in a sterile container after rinsing of the oral cavity with clean water. The collected specimens should be packaged and transported to the laboratory as soon as possible after collection.
Resources
- Guidelines for Programmatic Management of Tuberculosis Preventive Treatment, Central TB Division, MoHFW 2021
- Training Modules for Programme Managers and Medical Officers,Central TB Division, MoHFW 2020
- Guidelines on Airborne Infection Control, Directorate General of Health Services, MoHFW 2010
Assessment
Question Answer 1 Answer 2 Answer 3 Answer 4 Correct answer Correct explanation Page id Part of Pre-test Part of Post-test What are the key principles of TB diagnosis under NTEP?
Upfront testing for vulnerable groups Microbiological confirmation of all cases Good sample collection and transport All of the above
4 The key principles of TB diagnosis under NTEP are: microbiological confirmation for all cases, use upfront NAAT, quality sample collection and transport, and practicing universal precautions and AIC measures.
Biological Specimen for Diagnosis of TB
ContentFor laboratory diagnosis of TB, different biological specimens are used.
Pulmonary TB: Sputum sample is used. Sputum is a thick fluid produced in the lungs and in the adjacent airways. Normally, a spot sample and a fresh morning sample is preferred for the bacteriological examination of sputum.
Extra Pulmonary TB:
Resources:
Kindly provide your valuable feedback on the page to the link provided HERE
General process flow for testing in NTEP
ContentThe process for testing is initiated with a request for test and ends with the reporting of test results. In built into the process of testing is also the process of specimen collection and transportation.
1. Request for a test: This is the first step initiated when the requirement for a test is identified. This event is at the time of identification of presumptive TB/ DRTB, follow-up point (end of IP/CP, post treatment follow-up). The request may be initiated by the medical officer (MO) or the health staff at the Peripheral Health Institute (PHI) citing the reason for testing and the type of test required. The request is directed towards a laboratory where the required test is available. The request for test can be performed in Nikshay for any case that is already enrolled with an existing Patient ID. Requesting for test in Nikshay is analogous to filling up the physical request form Annexure 15A and generates a Test ID/ Test Request ID.
2. Patient Referral/ Sample collection and transportation: Following the request for test, the next step is to physically refer the patient to the corresponding laboratory, or collecting the appropriate biological sample and initiating its transportation to the lab. If biological sample is collected, the details of the sample need to be added under the request for test in Nikshay and the sample needs to be appropriately labelled and the corresponding details of the request test attached.
3. Performing the test: Once the sample has been received successfully at the destination laboratory, the lab technician (LT) updates the sample/ test record in Nikshay and initiates the relevant protocol for testing and follows through till results availability.
4. Reporting results: Once the results are available it needs to be updated against the corresponding request for a test and it is visible to all relevant stakeholders in Nikshay. If only Annexure 15A is available, the results need to be updated there and needs to be manually communicated to the personnel initiating the request for test.
Resources
- Training Modules for Programme Managers and Medical Officers
- Guidelines for Programmatic Management of Tuberculosis Preventive Treatment
Assessment
Question
Answer 1
Answer 2
Answer 3
Answer 4
Correct answer
Correct explanation
Page id
Part of Pre-test
Part of Post-test
Which of the following statements are correct?
Under NTEP, the process for testing is initiated with a request for test on only Nikshay.
Test requests for presumptive DR-TB cases are initiated only by specialists.
Test requests for all presumptive cases are initiated by the medical officer and/or other health staff at the Peripheral Health Institute (PHI).
All of the above
3
Test requests for all presumptive cases are initiated by the medical officer and/or other health staff at the Peripheral Health Institute (PHI).
Yes Yes Requesting a Test on Nikshay
ContentOnce a presumptive TB patient is identified, the patient is enrolled online by a healthcare worker or doctor in Nikshay online portal. For diagnosis of Tuberculosis, the treating physician can request a test utilizing the request test option of Nikshay online portal. The step-by-step approach for test request is as follows:
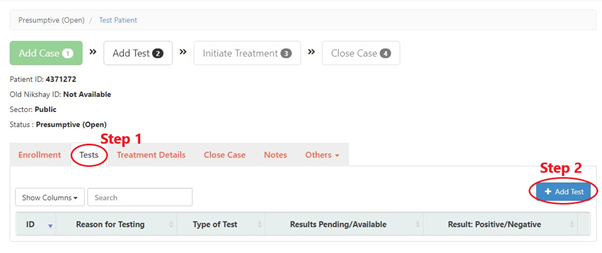
Step 0: Go to the Patients Page.
Step 1: Select the “Tests” tab.
Step 2: Click the “Add Test” button.
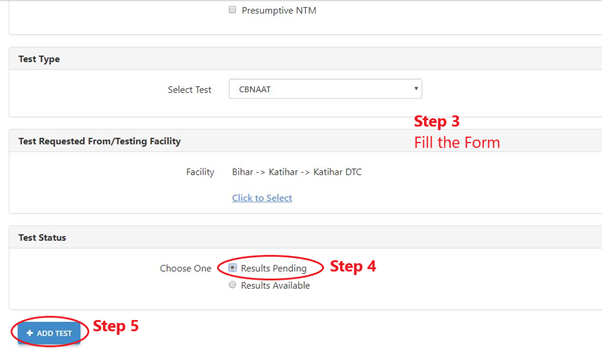
Step 3: Fill the form.
Step 4: Select the “Test Status” as “Results Pending”.
Step 5: Click the “Add Test” button by selecting the appropriate test for the patient.
In a situation where the patient is referred to another health facility for TB testing, one needs to select the test requested along with the facility name where the patient will visit for undergoing the TB test. the results are added by the concerned healthcare worker only after the test is conducted and the result is available.
In the absence of such results, it will show ‘Result pending’ instead of ‘Result available’ status.
Video fileVideo: Process to add tests on Ni-kshay
Resources
Kindly provide your valuable feedback on the page to the link provided HERE
Fullscreen